AI Subrogation Recovery Agent
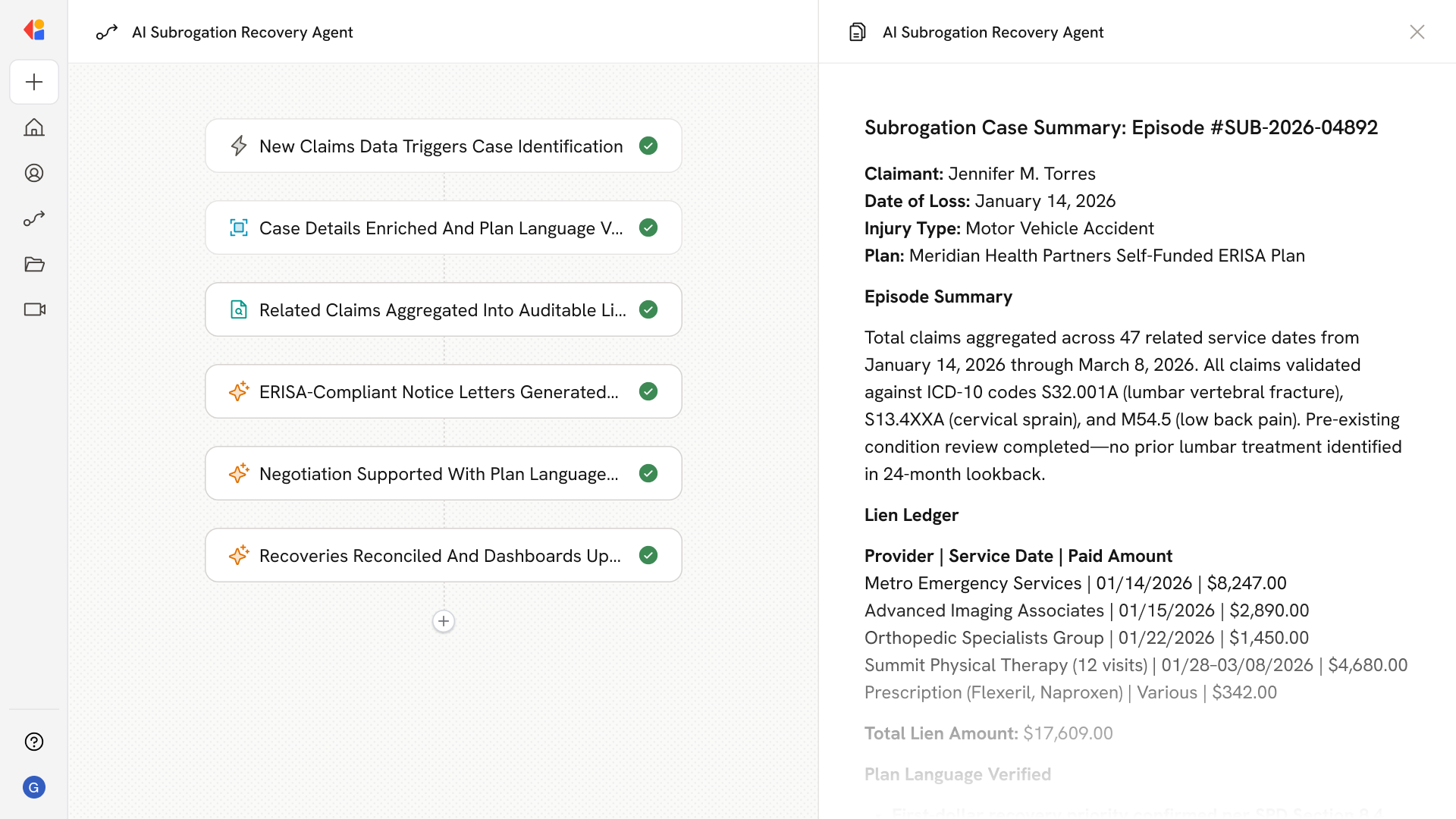
Automating Subrogation Recovery with AI
Real-Time Case Identification Without Member Questionnaires
The agent monitors claims data, ICD-10 external cause codes, and third-party sources to detect accident-related episodes as they occur eliminating reliance on low-return questionnaires while capturing cases that manual processes miss.
Dynamic Lien Management and Notice Automation
AI-driven workflows automatically compile and update lien values as claims post, generate ERISA-compliant notice letters, and track delivery to adverse carriers and plaintiff’s counsel securing the plan’s reimbursement position early.
Accelerated Cycle Time with Higher PMPY
Automated triage, relatedness review, and negotiation support compress the accident-to-cash timeline while maximizing recoveries per member per year through consistent first-dollar priority enforcement.
How Cassidy automates this using AI
Step 1: Trigger on new claims data
The Workflow activates when medical claims, 835/837 transactions, or ADT feeds arrive scanning ICD-10 codes, provider types, and place-of-service indicators to flag potential third-party liability cases in near real-time.
Step 2: Enrich and validate the case
Cassidy pulls from the Knowledge Base to verify plan language (first-dollar priority, made-whole disclaimers, equitable lien provisions), confirms self-funded ERISA status, and enriches the file with public records like police reports or workers’ comp databases.
Step 3: Build the episode and calculate the lien
The agent aggregates related claims across the injury episode, flags pre-existing conditions, and maintains a dynamic, auditable lien ledger that updates automatically as new claims post.
Step 4: Generate and send notice letters
Cassidy drafts ERISA-compliant reimbursement assertions including plan name, date of loss, and source of rights then routes them to adverse carriers, plaintiff’s counsel, and lien-resolution groups with certified delivery tracking.
Step 5: Support negotiation and settlement
The Workflow surfaces plan language, policy limit disclosures, and fee allocation calculators to guide negotiations. Human-in-the-Loop approval ensures final settlement terms align with fiduciary duties before fund disbursement.
Step 6: Reconcile and report
Once funds are received, Cassidy posts recoveries against paid claims, coordinates with stop-loss where applicable, and updates dashboards with PMPY, cycle time, and recovery-per-file metrics for continuous improvement.
Implement it inside your company
- Hands-on onboarding and support
- Self-paced training for your team
- Dedicated implementation experts
- Ongoing use case discovery
- ROI tracking & analytics dashboards
- Proven playbooks to get started fast



