AI Healthcare Financial Reconciliation Agent
Automating Healthcare Financial Reconciliation with AI
Automating ERA Intake & Matching
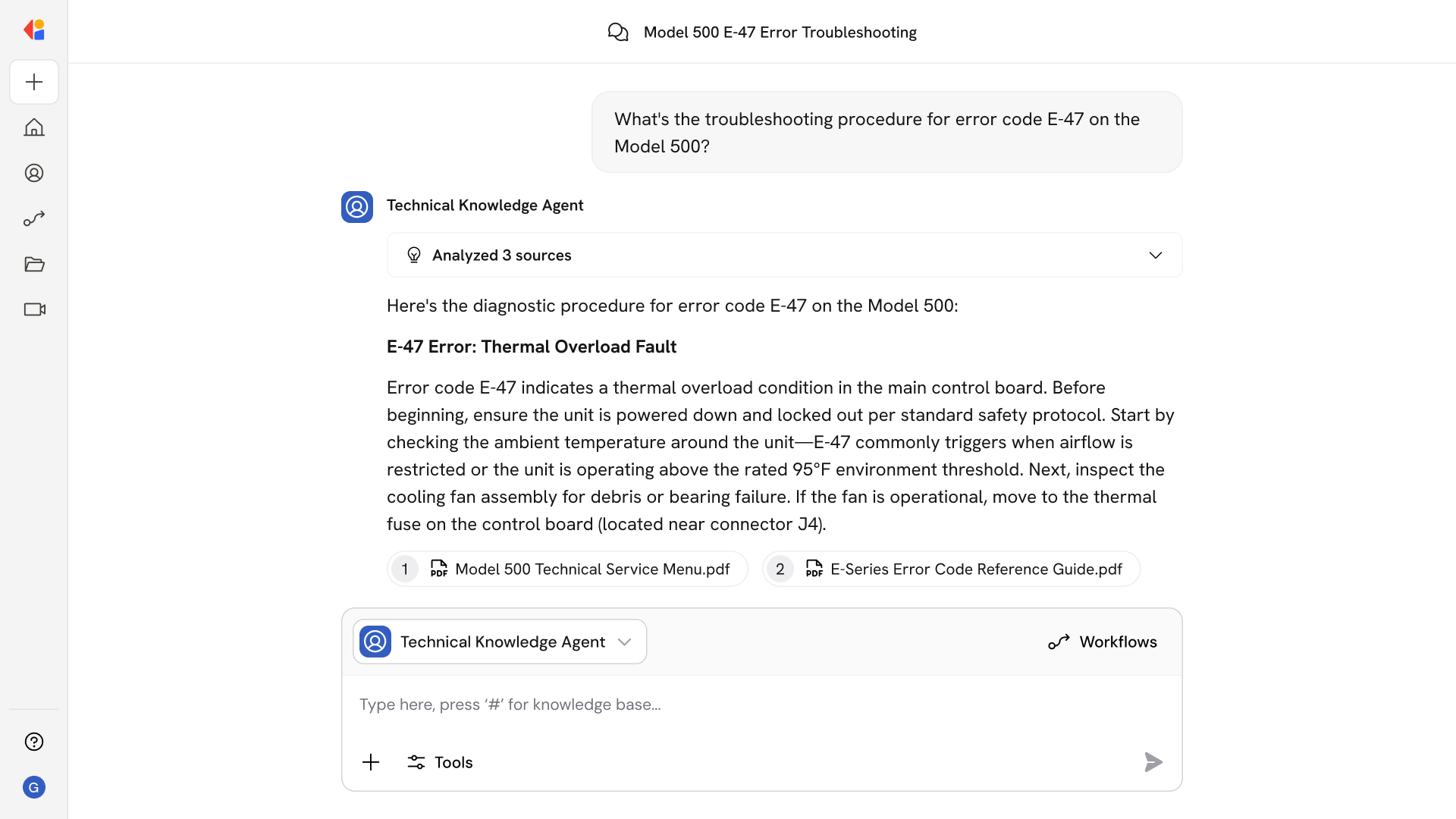
The agent automatically matches incoming ERA files to bank deposits using TRN trace numbers, confirming BPR02 amounts against ACH references and flagging mismatches for review.
Precision Claim and Adjustment Posting
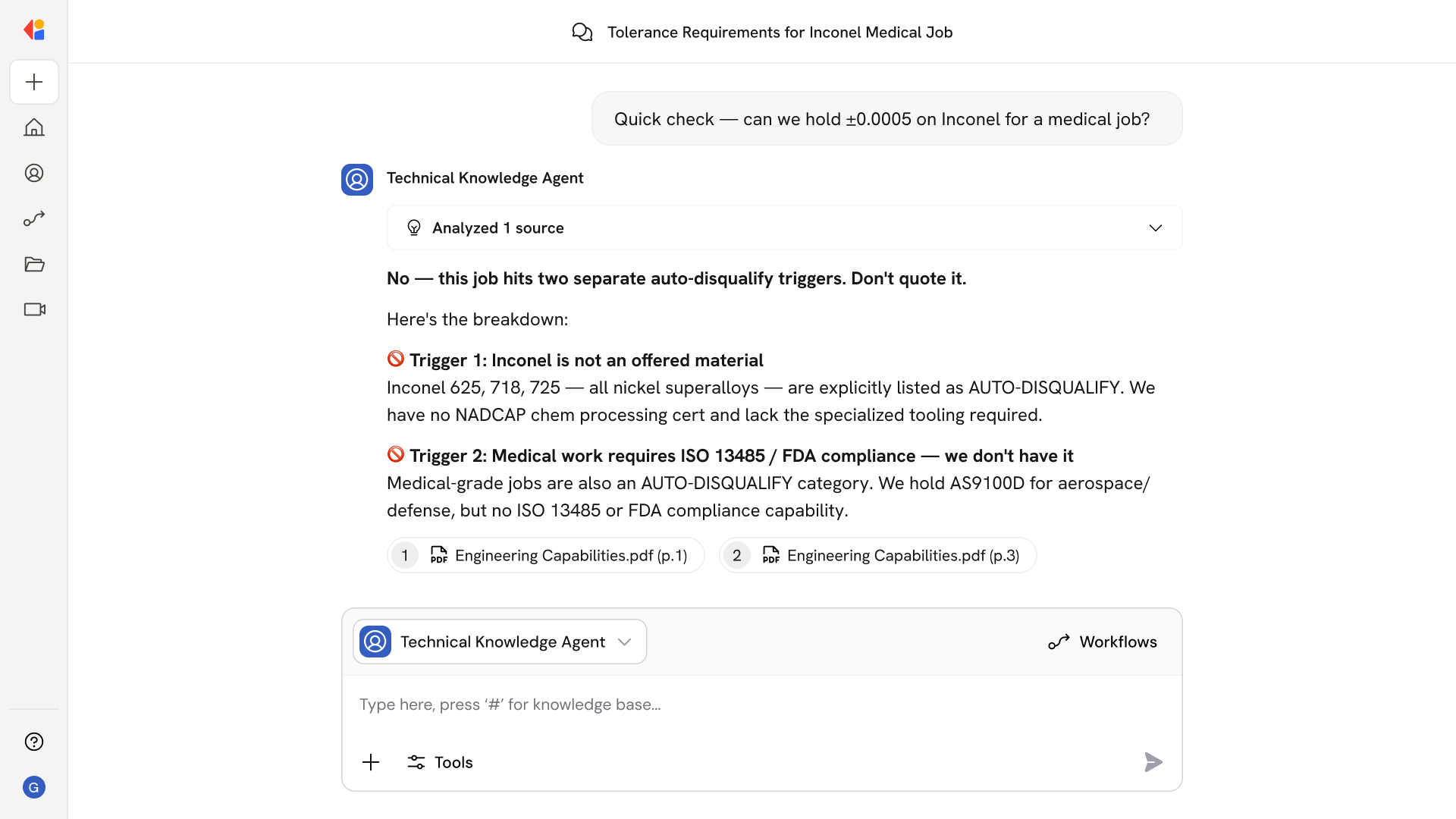
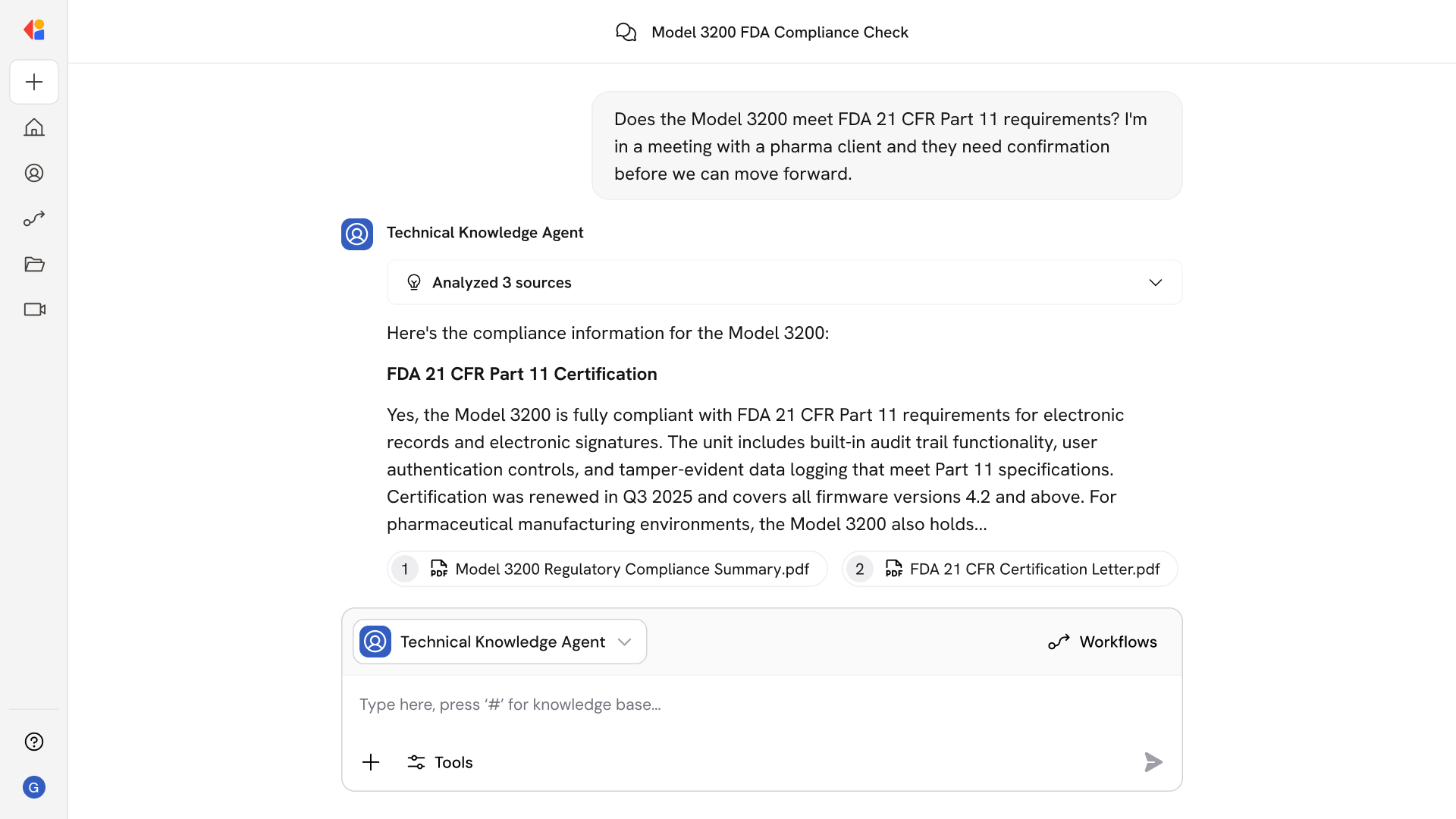
AI-driven automation posts claim-level payments (CLP/SVC) with accurate CARC/RARC-coded adjustments, correctly routing amounts to patient responsibility, contractual write-offs, and net paid balances.
Provider-Level Balance Controls
The system processes PLB entries for non-claim adjustments—recoupments, interest, and withholds—creating offsetting journal entries that ensure BPR02 balances against the sum of claims and provider-level adjustments.
How Cassidy automates this using AI
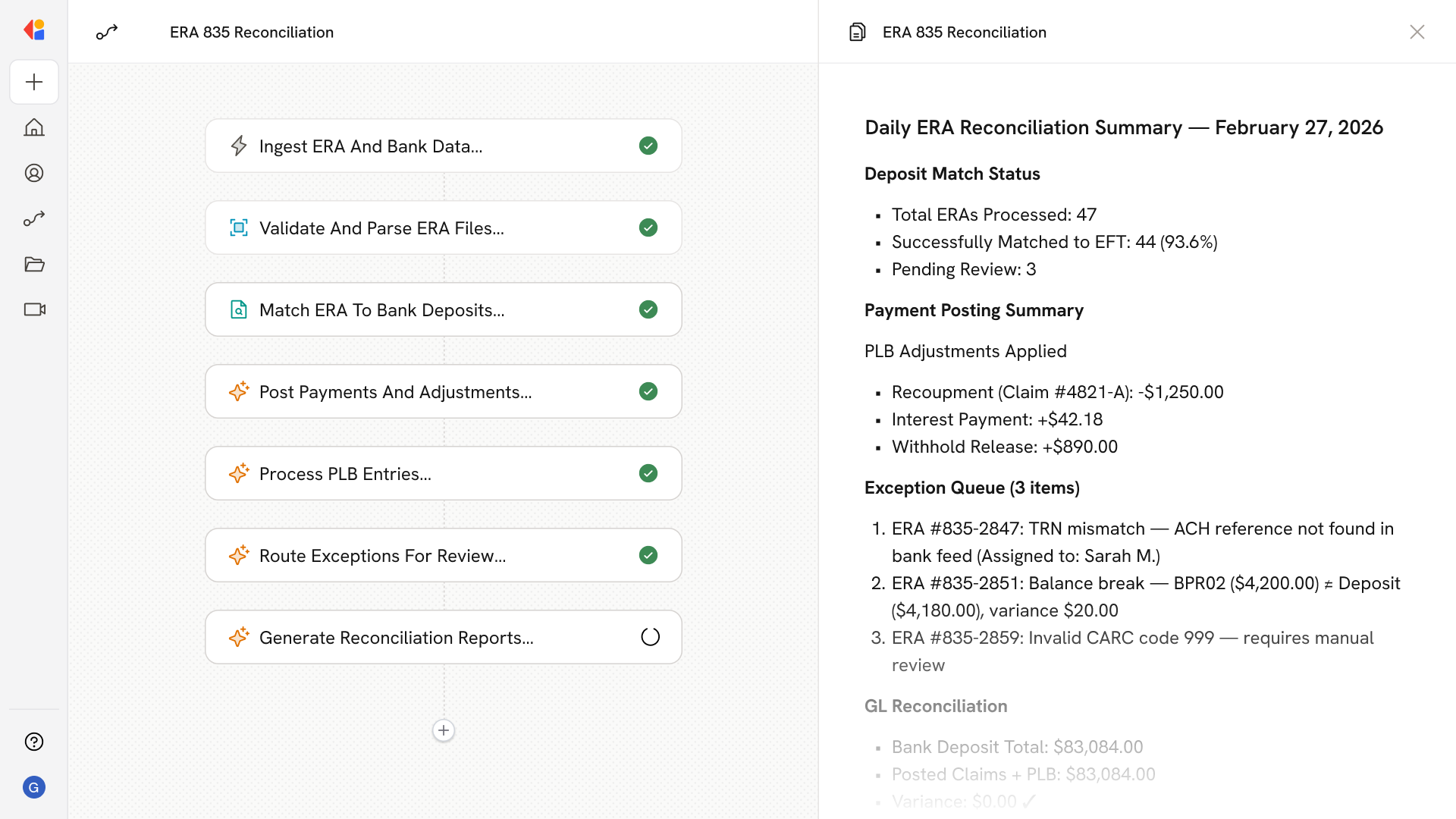
Step 1: Ingest ERA and bank data
The Workflow triggers when new ERA 835 files arrive via secure transport or clearinghouse connection, while simultaneously pulling EFT deposit data from bank feeds for reassociation.
Step 2: Validate and parse the ERA
Cassidy performs SNIP-style validation—checking envelope integrity (ISA/GS/ST), verifying CARC/RARC codes against national code sets, and confirming segment-level balancing rules per payer companion guides.
Step 3: Match ERA to bank deposit
The Workflow extracts TRN02 from each ERA and matches it to the corresponding ACH reference on the bank statement, confirming that BPR02 equals the deposited amount and queuing discrepancies for exception handling.
Step 4: Post payments and adjustments
Cassidy maps payer and provider identities, then posts CLP claim summaries and SVC service lines to your practice management system—applying CAS adjustments to update patient responsibility, write-offs, and net paid balances.
Step 5: Process PLB adjustments
The Workflow identifies provider-level balance entries (recoupments, interest, withholds) and creates offsetting journal entries, ensuring the final reconciliation balances BPR02 against posted claims plus PLB adjustments.
Step 6: Route exceptions for review
Items that fail validation—balance breaks, TRN mismatches, invalid codes, or zero-pay remittances—are automatically queued with root-cause categorization for your team to remediate.
Step 7: Generate reconciliation reports
Cassidy produces audit-ready reports showing ERA-to-EFT matches, PLB entries, outstanding exceptions, and GL summaries—giving your team complete visibility from bank deposit to posted claim.
Implement it inside your company
- Hands-on onboarding and support
- Self-paced training for your team
- Dedicated implementation experts
- Ongoing use case discovery
- ROI tracking & analytics dashboards
- Proven playbooks to get started fast