AI Medical Coding Audit Agent
Automating Medical Coding Audits with AI
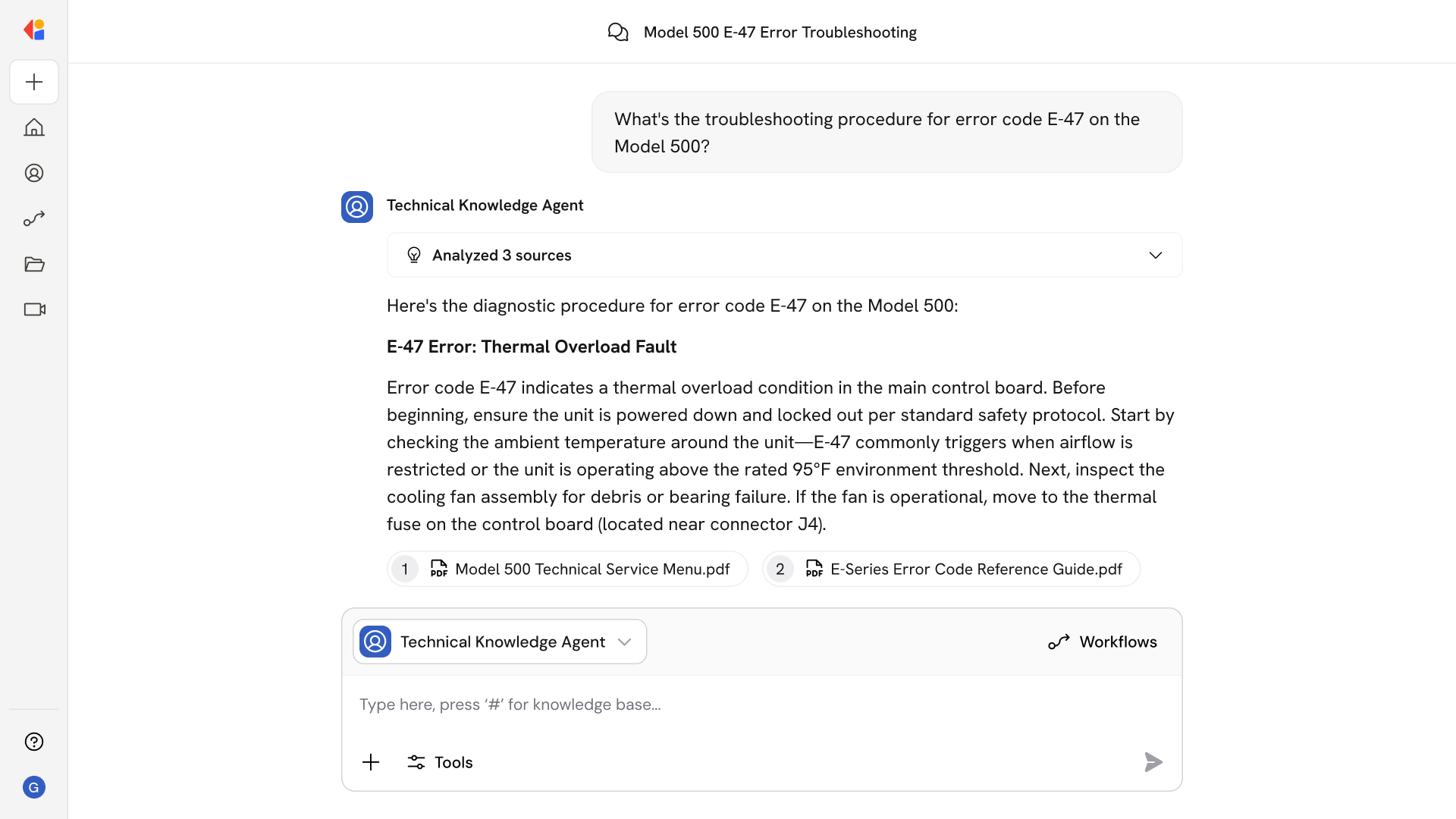
Analyze 100% of encounters pre-bill
Move beyond sample-based audits to review every encounter before claim submission, using rules engines and ML to detect DRG shifts, bundling violations, modifier omissions, and medical necessity gaps that cause denials.
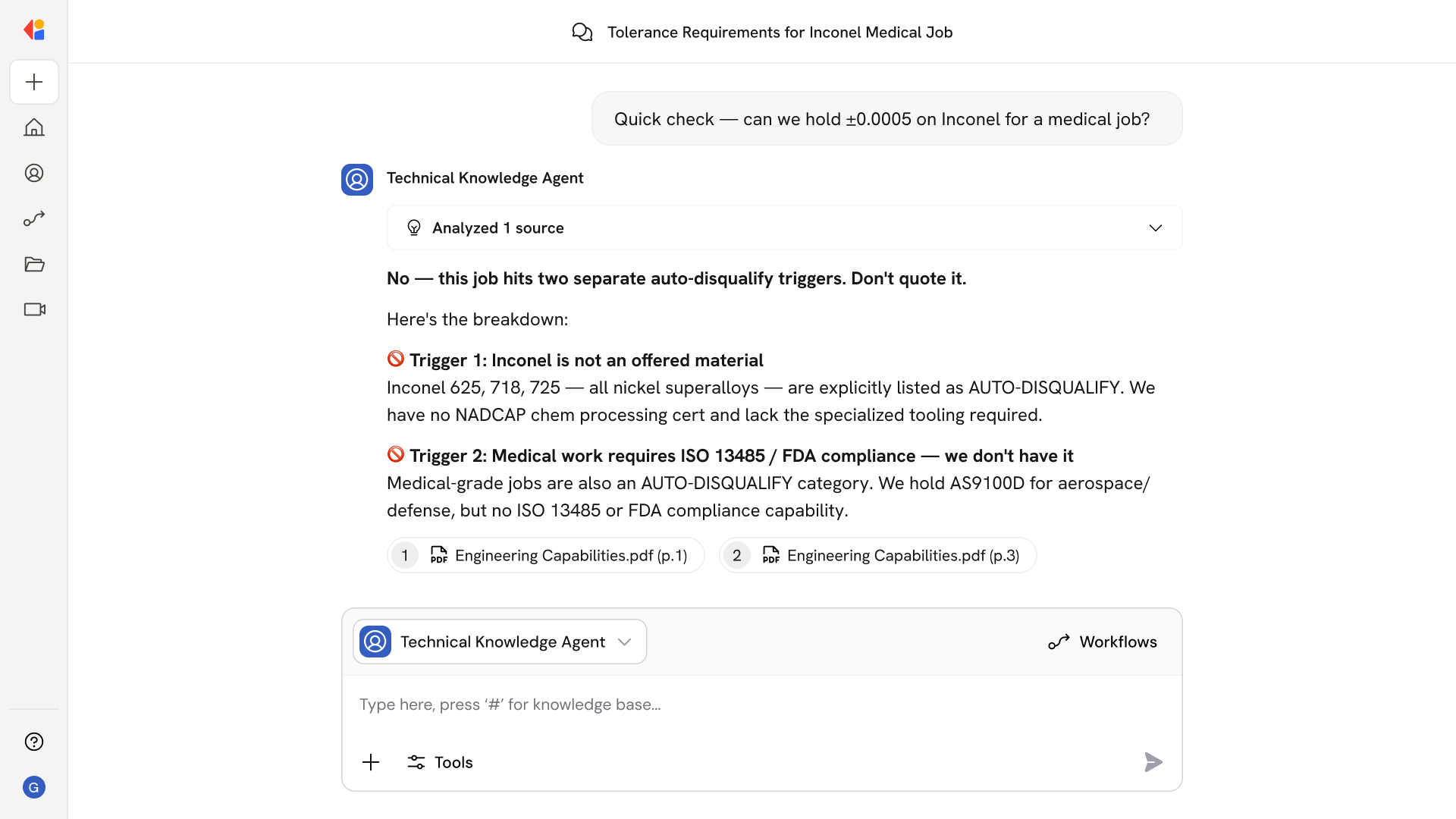
Surface actionable variance insights with financial impact
The agent compares coding against clinical documentation, grouper results, NCCI edits, and payer-specific policies—then quantifies each variance by dollar impact and denial risk so teams can prioritize high-value corrections.
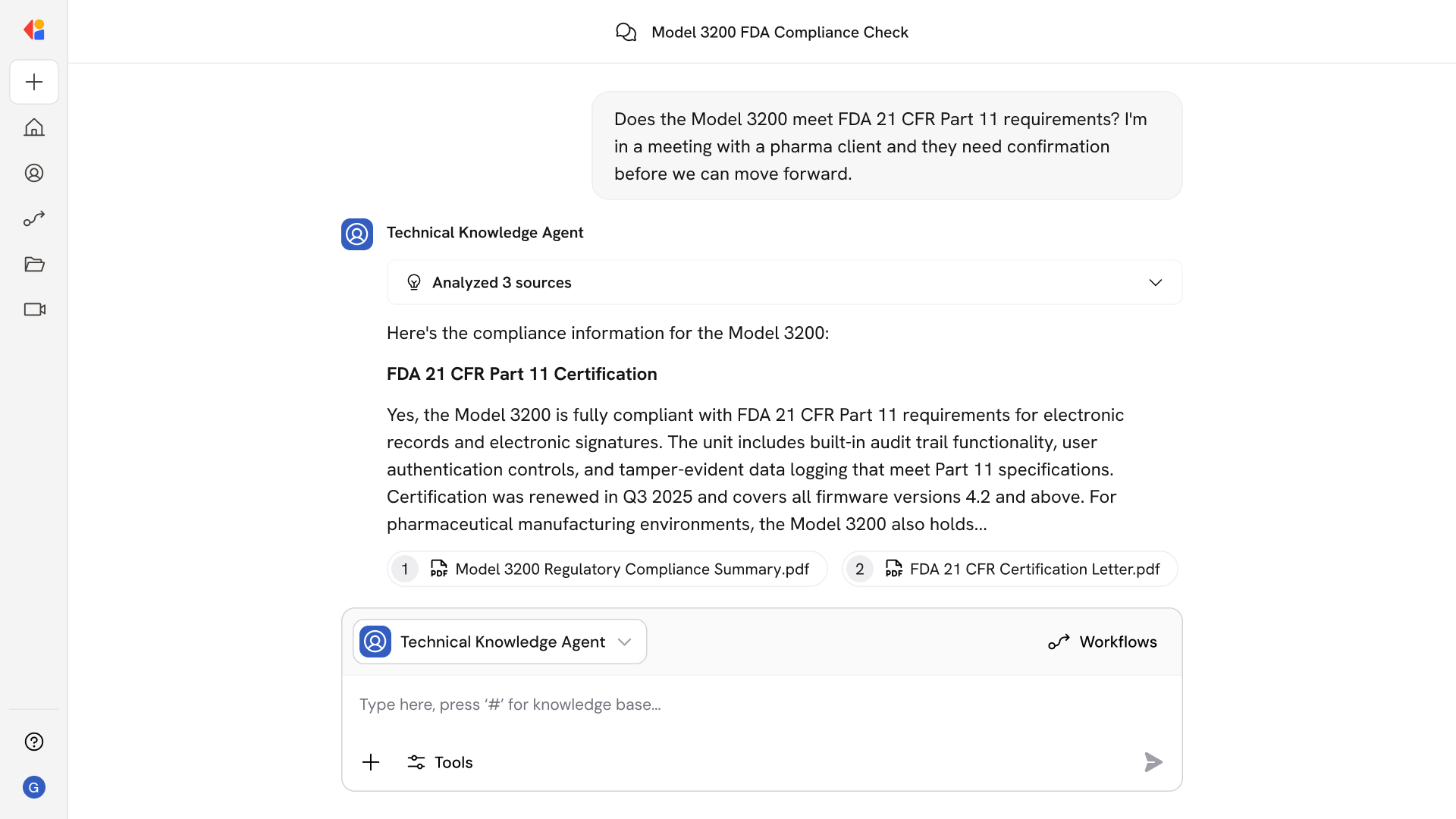
Route flagged encounters to the right reviewer automatically
Role-based queues direct variances to coders, CDI specialists, or compliance teams with encounter-specific guidance, reducing manual triage and ensuring clean claims go out on first pass.
How Cassidy automates this using AI
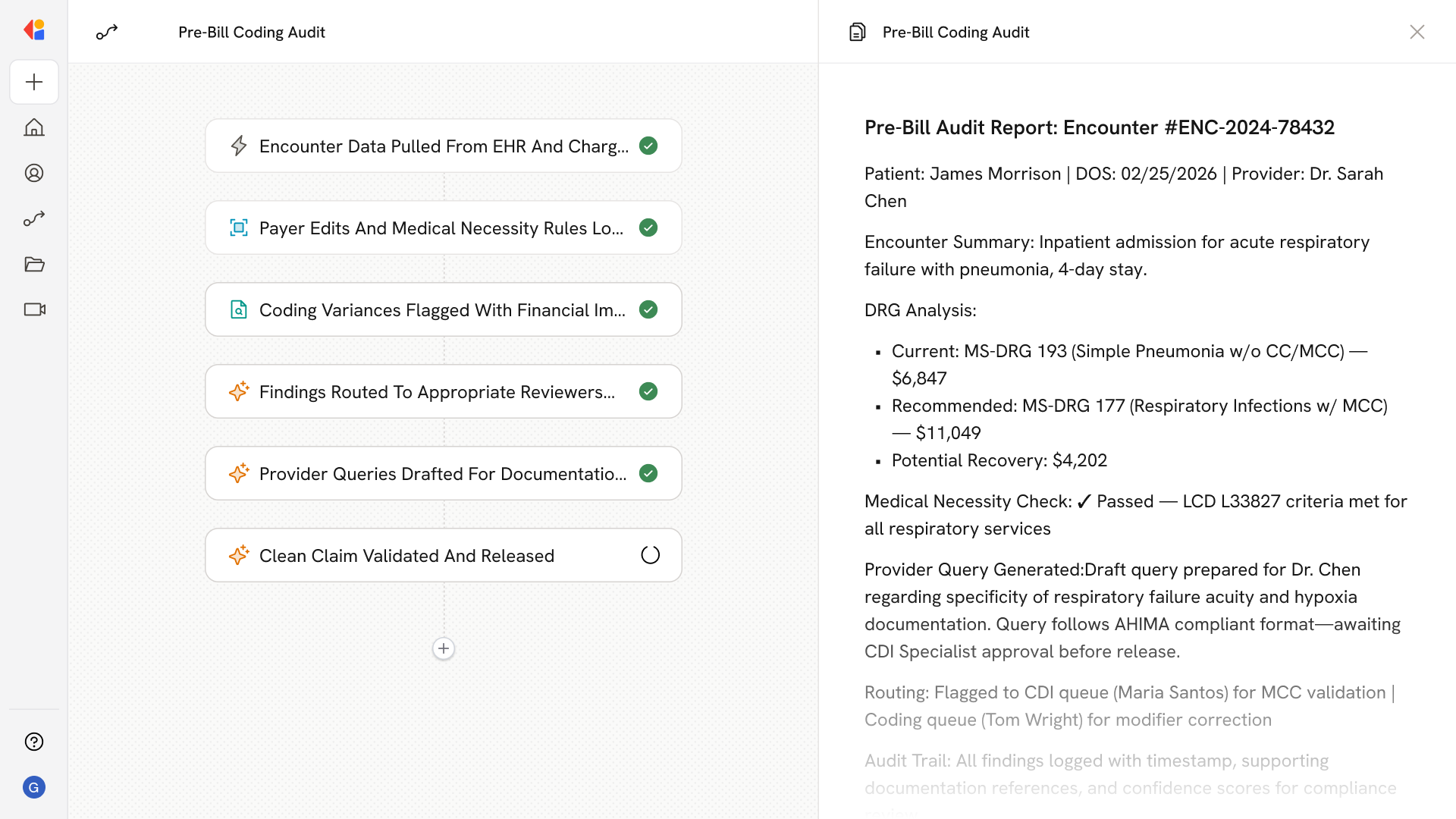
Step 1: Trigger on encounter ready for billing
The Workflow activates when an encounter reaches the pre-bill queue—pulling structured and unstructured data from the EHR, encoder/grouper outputs, charge capture systems, and current code sets (ICD-10-CM/PCS, CPT, HCPCS).
Step 2: Ingest payer edit libraries and policies
Cassidy pulls NCCI PTP/MUE edits, LCD/NCD rules, payer-specific medical necessity policies, and prior authorization flags from your Knowledge Base to ensure audits reflect current requirements.
Step 3: Run variance analysis against encounter context
The AI analyzes coding against clinical documentation, grouper results, and payer rules—flagging potential DRG changes, CC/MCC capture gaps, bundling conflicts, modifier needs, HCC opportunities, and medical necessity risks with confidence ratings and estimated financial impact.
Step 4: Route flagged encounters with actionable guidance
Cassidy auto-routes variances to coders, CDI specialists, or compliance reviewers through role-based queues, providing encounter-specific recommendations and supporting documentation references to accelerate resolution.
Step 5: Generate compliant provider queries when needed
For documentation insufficiencies, Cassidy drafts provider queries aligned to AHIMA/ACDIS standards—ready for Human-in-the-Loop review before sending to physicians.
Step 6: Confirm clean claim and release
After corrections, Cassidy re-runs payer edit checks to validate the encounter passes all rules, then releases the claim for submission with a complete audit trail for compliance documentation.
Implement it inside your company
- Hands-on onboarding and support
- Self-paced training for your team
- Dedicated implementation experts
- Ongoing use case discovery
- ROI tracking & analytics dashboards
- Proven playbooks to get started fast