AI Physician Credentialing Agent
Automating Physician Credentialing with AI
Real-Time Primary Source Verification
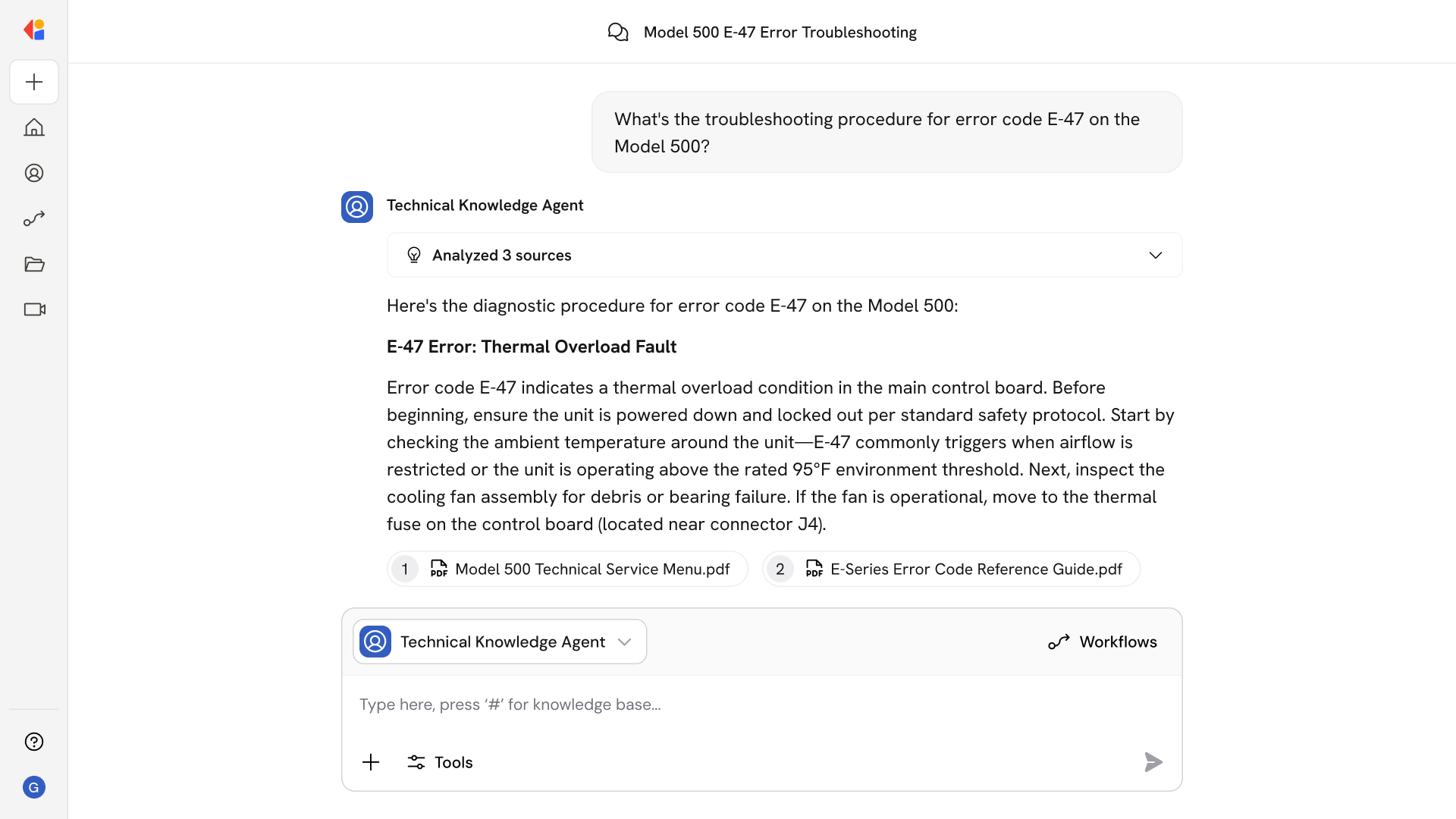
The agent automatically verifies licenses, DEA registrations, board certifications, and sanctions status directly from authoritative sources—state boards, ABMS, OIG LEIE, and NPDB—eliminating manual lookups and ensuring verification aging windows are met.
Streamlined Payer Enrollment
AI automation handles Medicare PECOS submissions, Medicaid applications, and commercial payer enrollments in parallel, tracking submission statuses and effective dates to accelerate time-to-revenue.
Continuous NCQA Compliance Monitoring
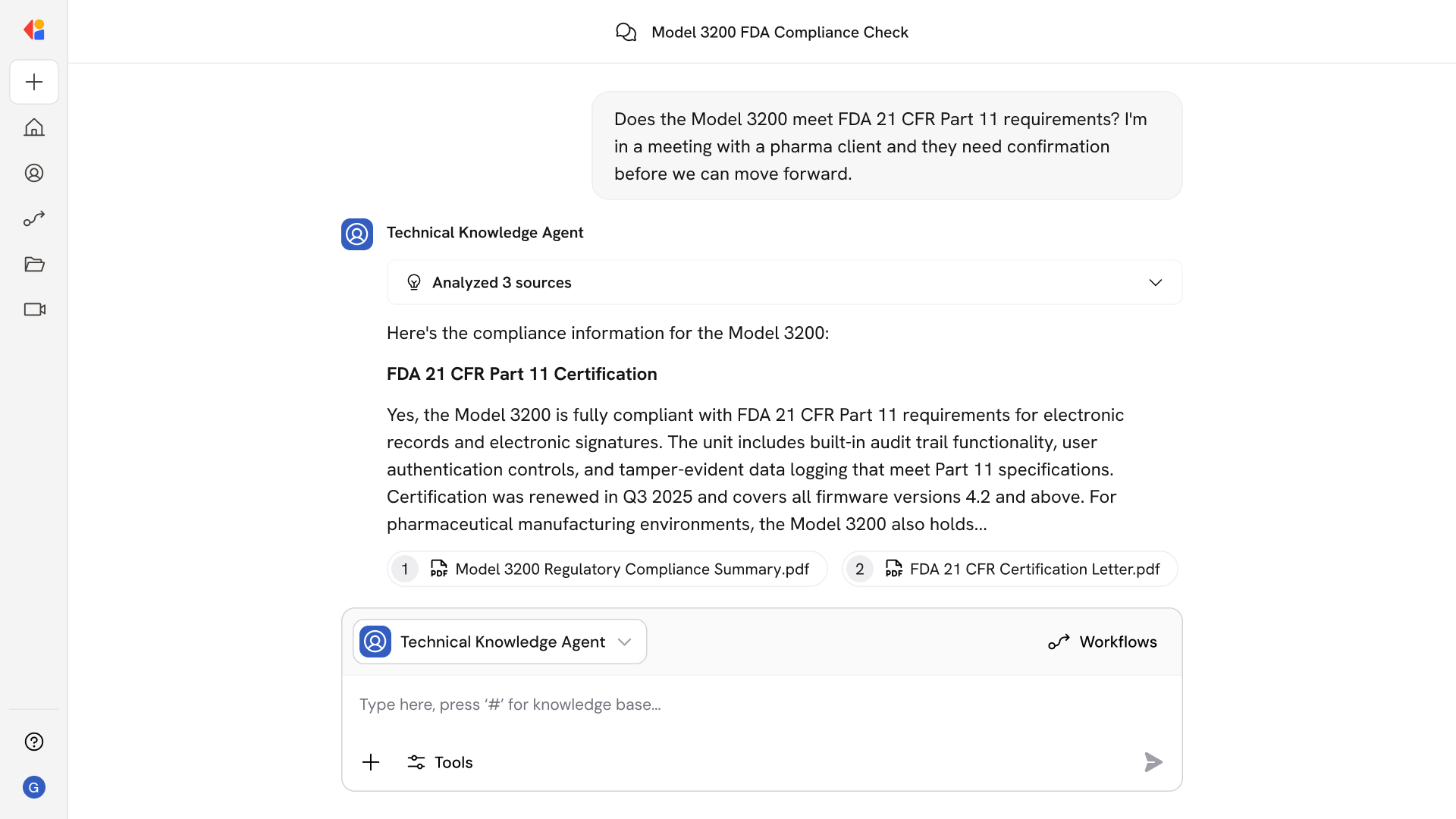
Automated workflows enforce CR 1–CR 8 standards, manage expirables with proactive alerts, generate audit-ready documentation, and maintain ongoing sanction monitoring between recredentialing cycles.
How Cassidy automates this using AI
Step 1: Intake and profile assembly
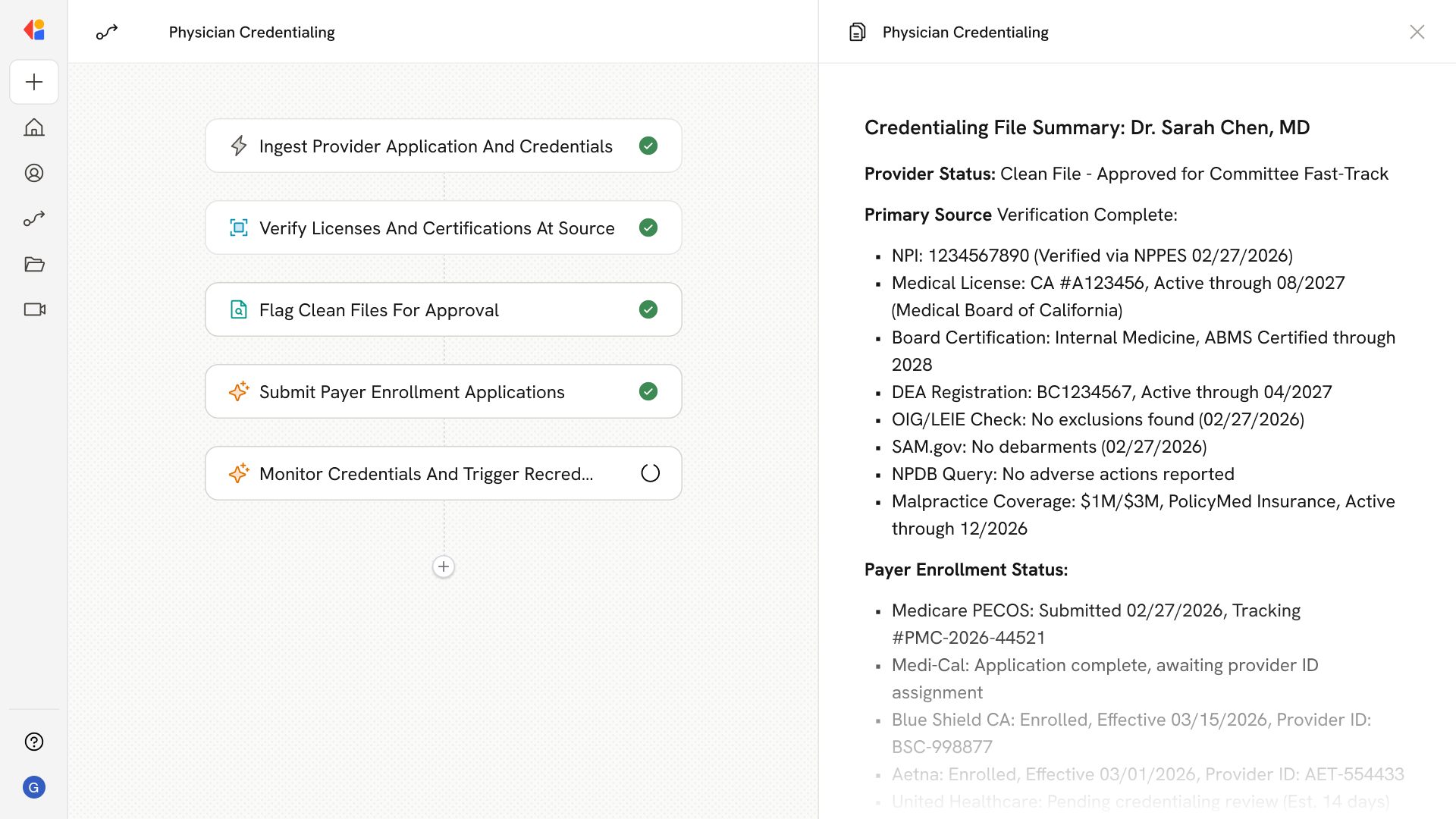
The Workflow triggers when a new provider application is submitted or pulled from CAQH ProView. Cassidy automatically ingests NPI/NPPES data, demographics, education, training history, licenses, DEA registrations, board certifications, malpractice coverage, and signed attestations into a unified credentialing file.
Step 2: Automated primary source verification
Cassidy executes PSV checks across all required elements—querying state licensing boards, ABMS for board certification, OIG LEIE and SAM.gov for sanctions, NPDB for malpractice history, and DEA databases. Each verification is date-stamped and stored with source documentation to meet 180/365-day aging requirements.
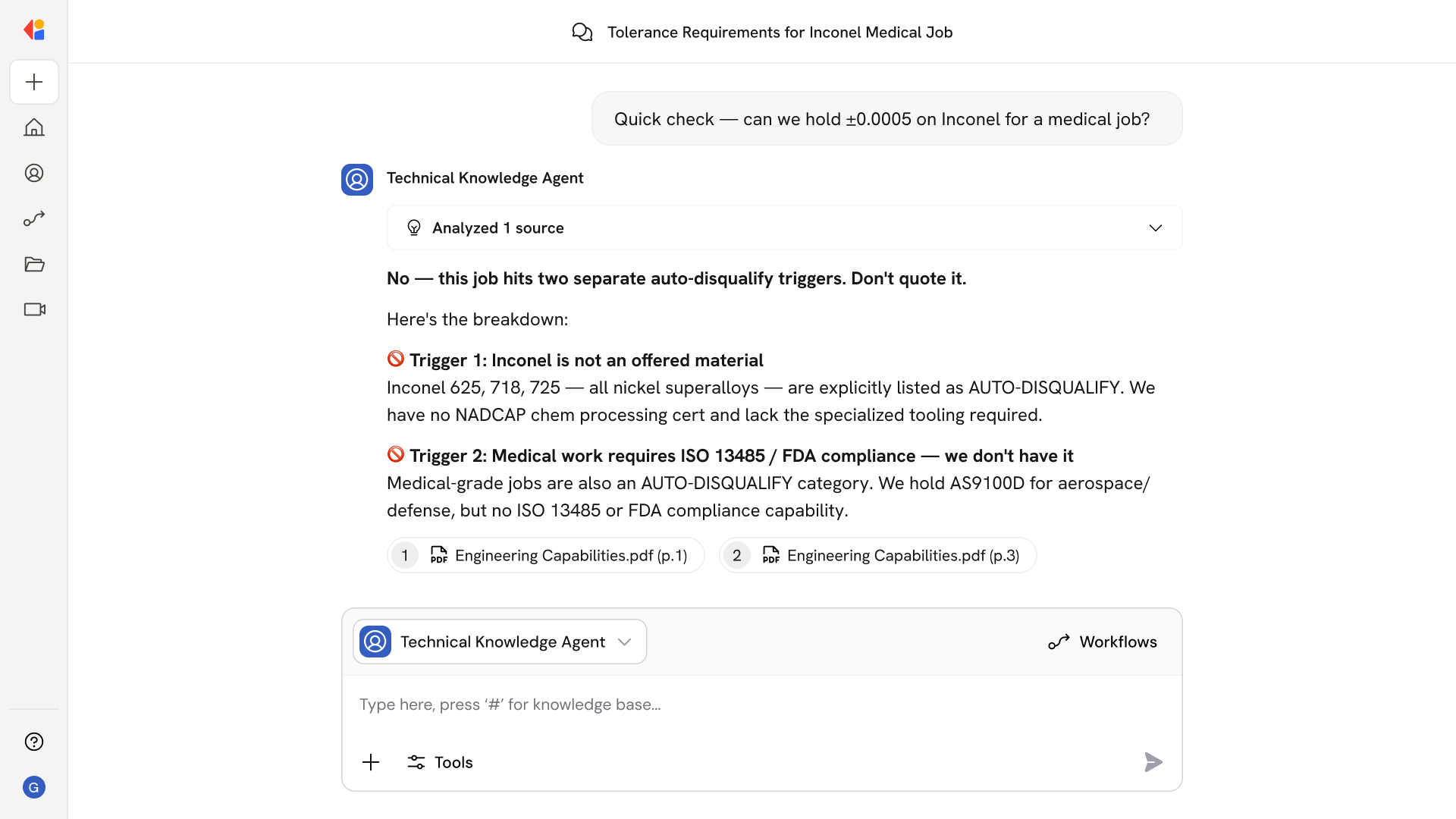
Step 3: Clean file determination and committee routing
The Workflow applies your organization's policy rules to determine clean file status. Clean files route to medical director approval; non-clean files generate committee packets with PSV artifacts, red flags, and summaries for Credentialing Committee review.
Step 4: Payer enrollment execution
Upon credentialing approval, Cassidy initiates parallel payer enrollment—submitting Medicare applications through PECOS, completing state Medicaid portals, and populating commercial payer applications from CAQH data. The system tracks each submission status and captures payer IDs and effective dates.
Step 5: Ongoing monitoring and recredentialing
Cassidy continuously monitors for license status changes, new sanctions, board certification updates, and expiring credentials. Automated alerts trigger before expirations, and the system initiates recredentialing Workflows at the three-year mark to maintain uninterrupted compliance.
Implement it inside your company
- Hands-on onboarding and support
- Self-paced training for your team
- Dedicated implementation experts
- Ongoing use case discovery
- ROI tracking & analytics dashboards
- Proven playbooks to get started fast