AI Insurance EOB Extraction Agent
Automating EOB Extraction with AI
Accurate data capture from any remittance format
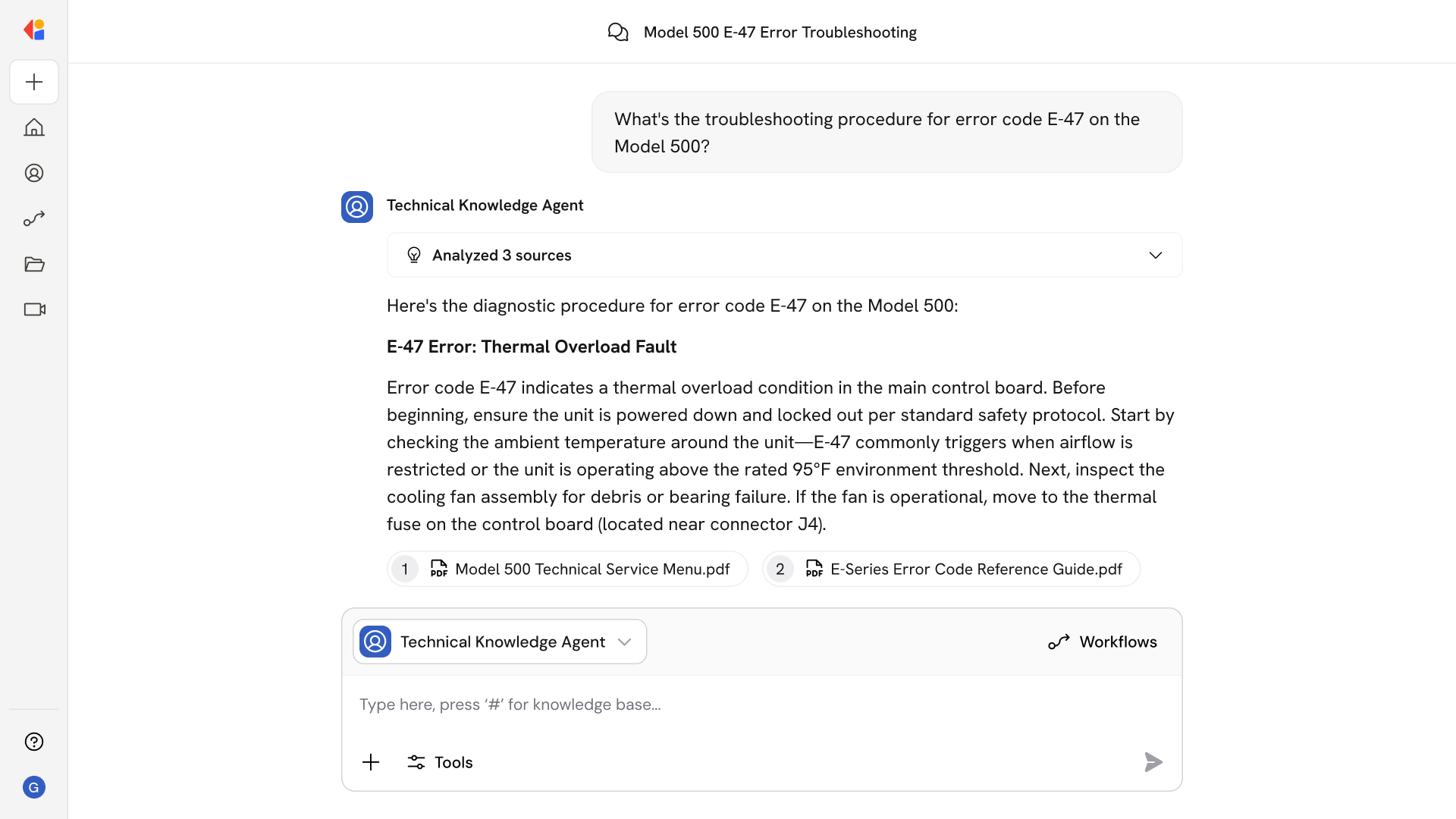
Accurate extraction across thousands of payer formats: The agent handles the variability of EOB layouts—paper, PDF, fax, lockbox images—and extracts header, claim, and line-level data with field-level confidence scoring and targeted human review for low-confidence values.
Standards-compliant 835 generation with CARC/RARC mapping: AI automation normalizes payer-specific reason text to official Claim Adjustment Reason Codes and Remittance Advice Remark Codes, constructs X12 005010X221A1-compliant ERAs, and enforces balancing rules across SVC, CLP, and BPR segments.
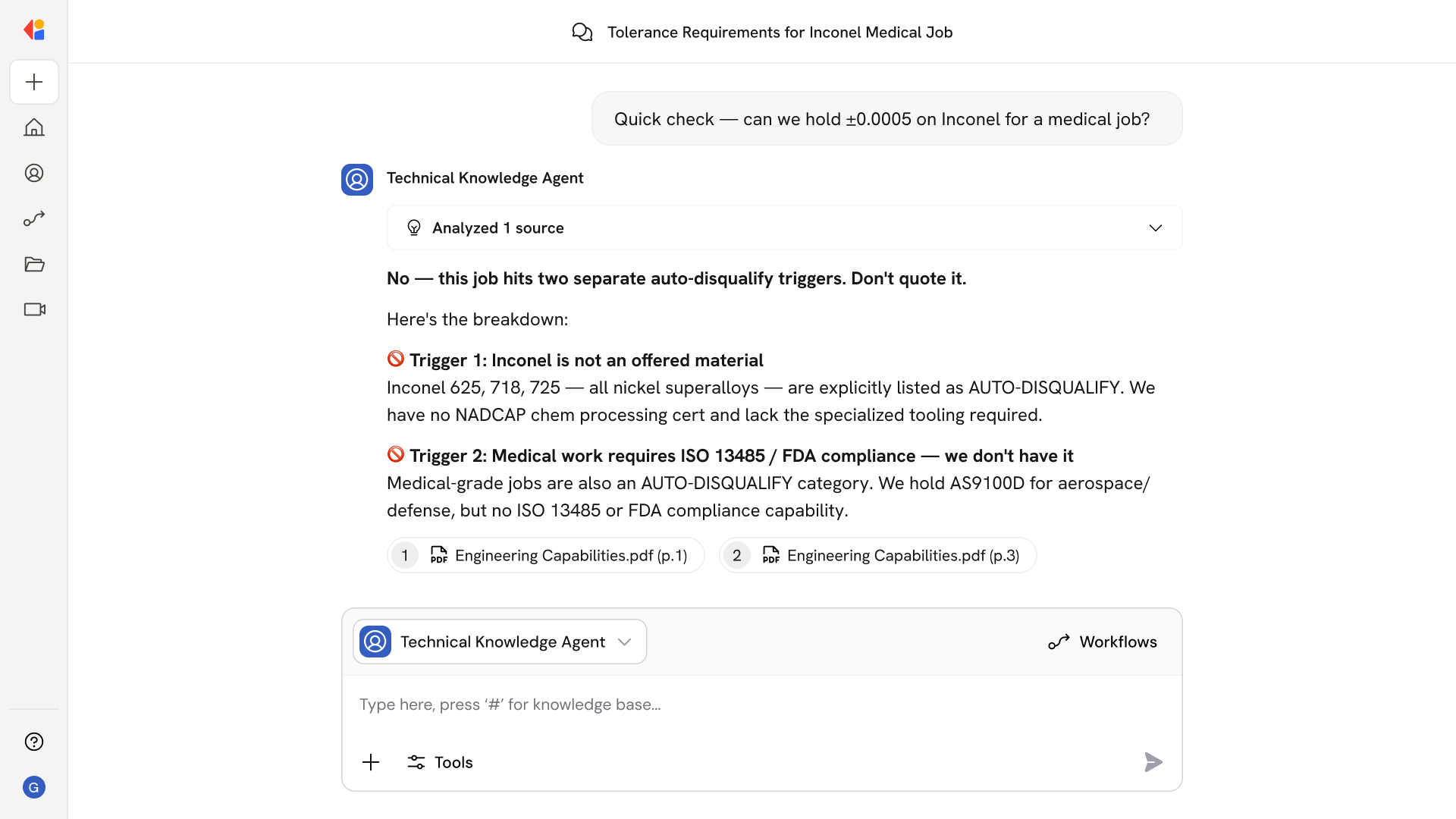
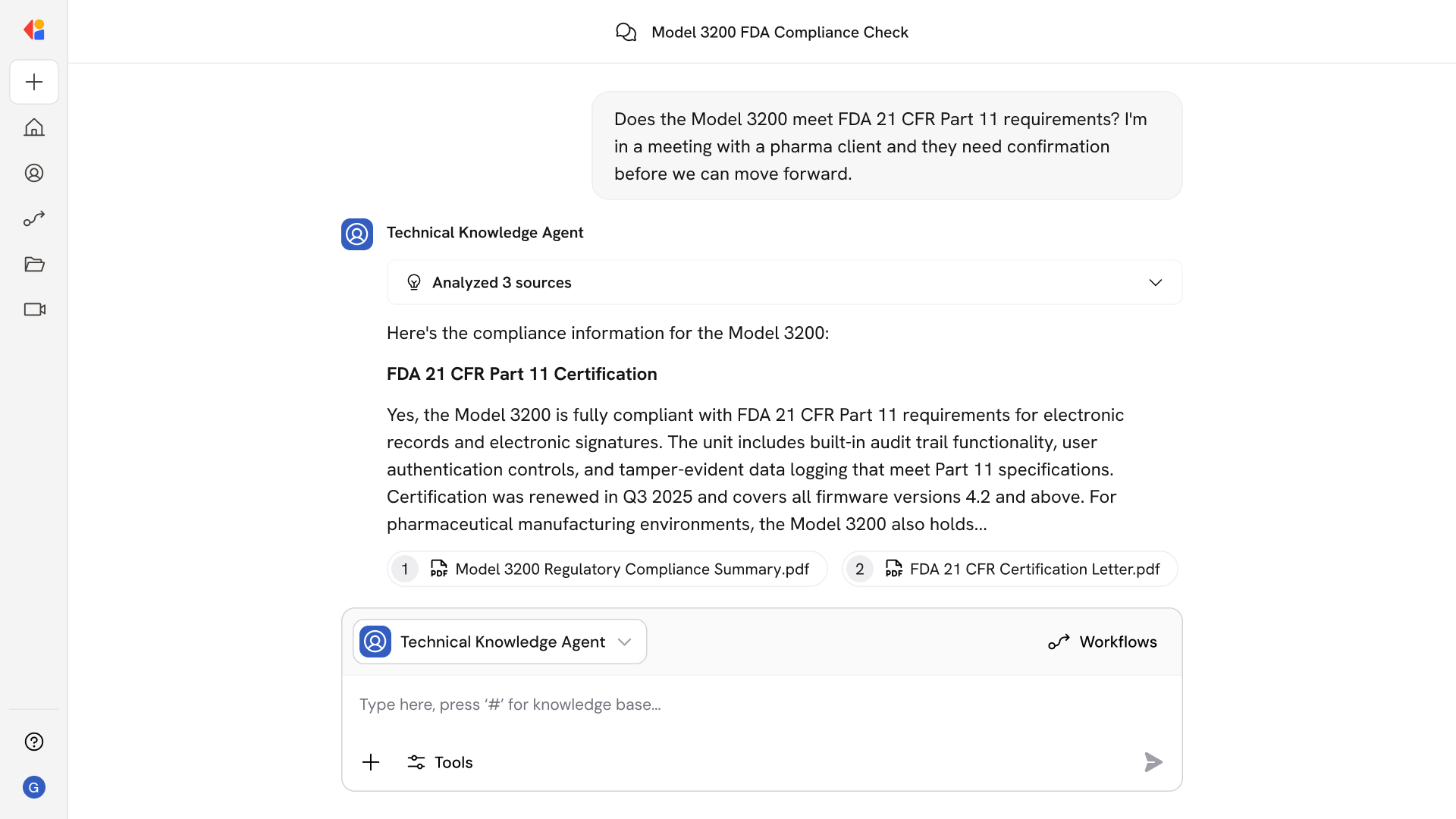
HIPAA-safe processing with human-in-the-loop controls: Automated workflows maintain full encryption, audit trails, and access controls for ePHI while routing exceptions—imbalances, unknown codes, PLB edge cases—to QA queues for review before posting.
How Cassidy automates this using AI
Step 1: Ingest EOB documents from any source
The Workflow triggers when new EOBs arrive—whether from a bank lockbox, SFTP drop, payer portal download, or scanned mail. Cassidy captures metadata (deposit date, check/EFT number, payer, amount) and classifies each document as EOB, denial letter, or correspondence.
Step 2: Pre-process and extract structured data
Cassidy applies de-skew, de-noise, and layout-aware OCR to extract header-level fields (payer ID, payee NPI, check number, totals), claim-level data (patient ID, payer claim control number, claim status), and line-level details (CPT/HCPCS, DOS, billed/allowed/paid amounts, adjustment text).
Step 3: Normalize codes and map to CARC/RARC
The Workflow aligns payer-specific reason text and proprietary codes to standardized CARC and RARC values, assigns correct group codes (CO, PR, OA, PI), and structures adjustments into CAS segments with proper LQ and MIA/MOA references per payer companion guides.
Step 4: Construct and validate the 835 ERA
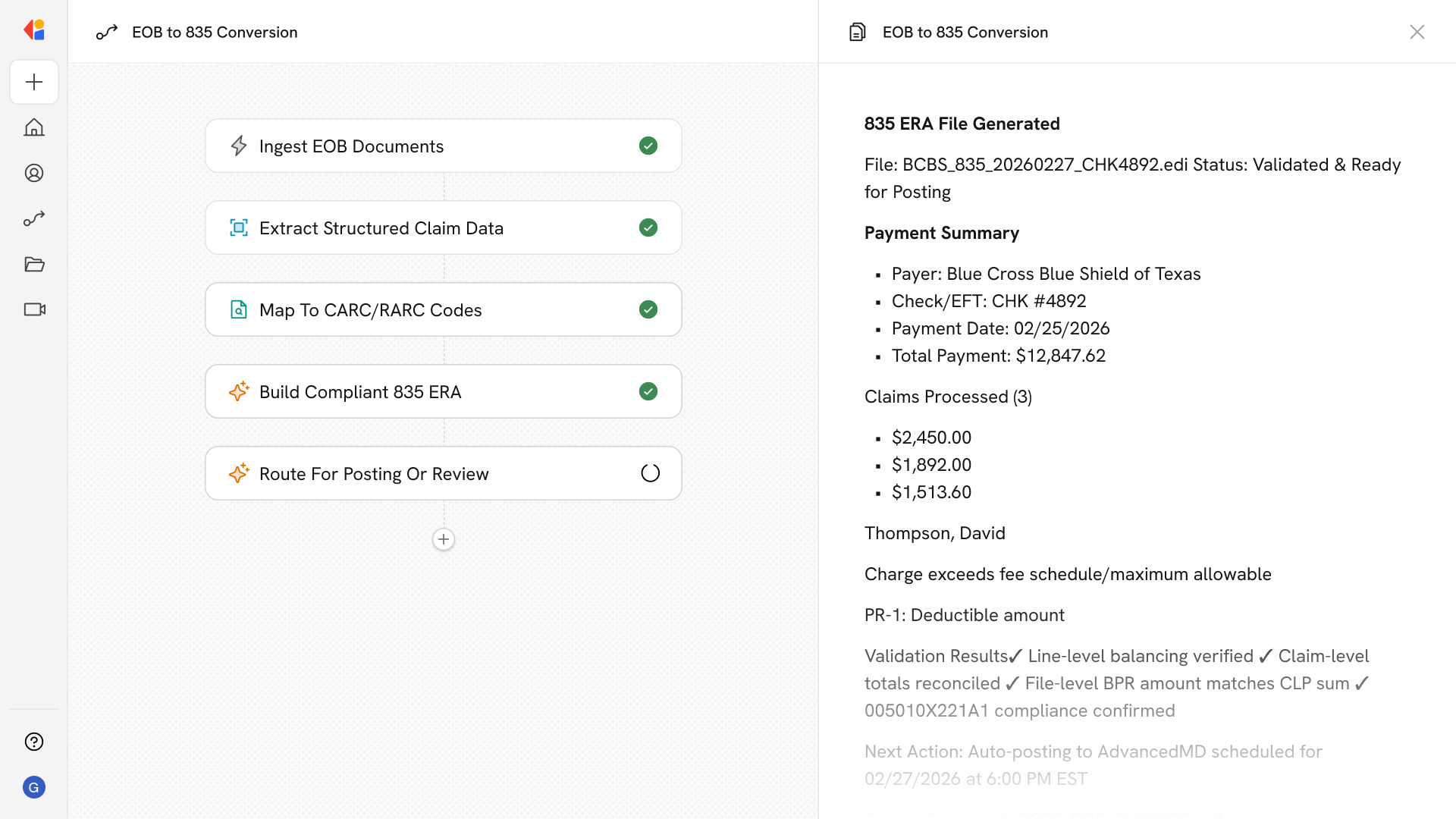
Cassidy builds a standards-compliant 005010X221A1 file—BPR payment header, TRN trace segments, CLP/SVC loops with CAS adjustments, and PLB entries for provider-level balancing. Built-in validation checks line/claim/file balancing and flags exceptions before output.
Step 5: Route for posting or human review
High-confidence ERAs flow directly to your PM/billing system for auto-posting at the line level. Low-confidence extractions, balancing discrepancies, or PLB edge cases route to a QA queue with Human-in-the-Loop approval—complete with audit trails and original document references.
Implement it inside your company
- Hands-on onboarding and support
- Self-paced training for your team
- Dedicated implementation experts
- Ongoing use case discovery
- ROI tracking & analytics dashboards
- Proven playbooks to get started fast