AI Healthcare Policy Search Agent
Automating Healthcare Policy Search with AI
Instant Policy Retrieval Across Payers and Products
The agent indexes and normalizes medical policies, coverage determinations, and clinical policy bulletins from commercial payers, Medicare NCDs/LCDs, and specialty benefit managers—so the right criteria surface in seconds, not hours of portal hunting.
Automated Criteria Extraction and Code Crosswalking
AI parses policy language to extract medical necessity requirements, step therapy rules, site-of-care restrictions, and documentation elements, then maps them to the exact CPT/HCPCS, ICD-10, and modifier combinations for the clinical scenario.
Documentation Checklists That Match Payer Language
The system generates patient-specific checklists aligned with policy verbiage—capturing prior treatment history, lab results, clinical scores, and specialist involvement—so submissions meet medical necessity standards on the first attempt.
How Cassidy automates this using AI
Step 1: Trigger on coverage inquiry
The Workflow activates when a user submits a coverage question—whether through Slack, Teams, or a browser extension—including the patient's payer, plan type, and planned service or drug.
Step 2: Identify payer, product, and benefit line
Cassidy determines the correct plan variation (commercial, Medicare Advantage, Medicaid, state, employer group) and whether the service falls under medical or pharmacy benefit to ensure the right policies apply.
Step 3: Search the Knowledge Base for governing policies
Cassidy queries your centralized Knowledge Base—containing indexed payer medical policies, NCDs, LCDs, LCAs, and specialty manager criteria like InterQual or MCG—to retrieve all applicable coverage documentation.
Step 4: Extract criteria and map to clinical scenario
The Agent parses policy language to identify medical necessity criteria, indications, contraindications, step therapy requirements, quantity limits, and site-of-care rules, then crosswalks them to the relevant CPT/HCPCS, ICD-10, and modifier codes.
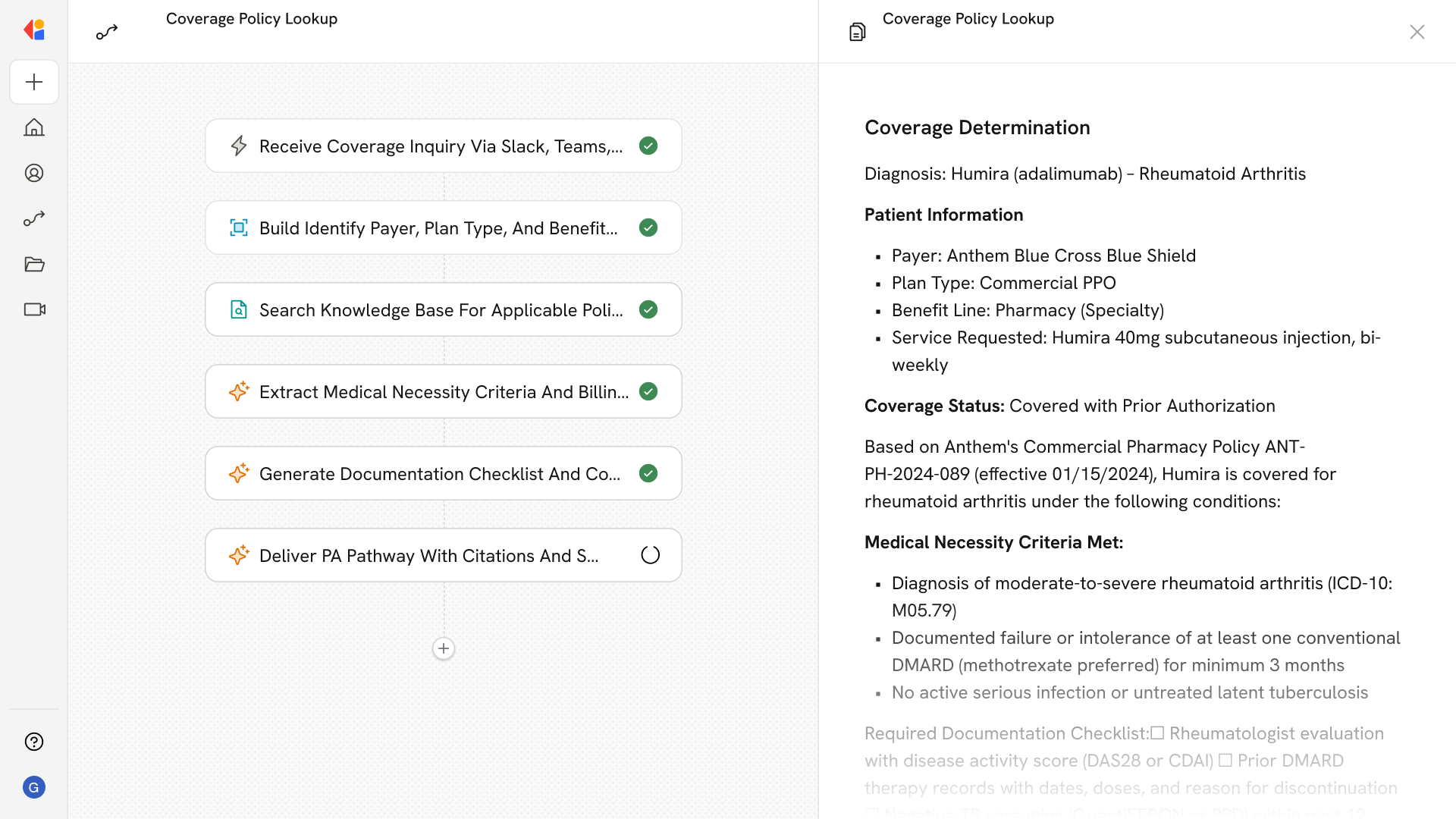
Step 5: Generate documentation checklist and coverage summary
Cassidy produces a structured checklist of required clinical elements—diagnosis confirmation, prior treatment outcomes, imaging results, specialist involvement—along with a clear coverage determination summary and rationale.
Step 6: Recommend PA pathway and deliver results
The Workflow identifies the correct submission channel (payer portal, X12 278, FHIR PAS, or ePA) and delivers the policy packet, checklist, and billing guidance directly to the user with citations to source policies and version dates.
Implement it inside your company
- Hands-on onboarding and support
- Self-paced training for your team
- Dedicated implementation experts
- Ongoing use case discovery
- ROI tracking & analytics dashboards
- Proven playbooks to get started fast