AI FSA HSA Claim Processing Agent
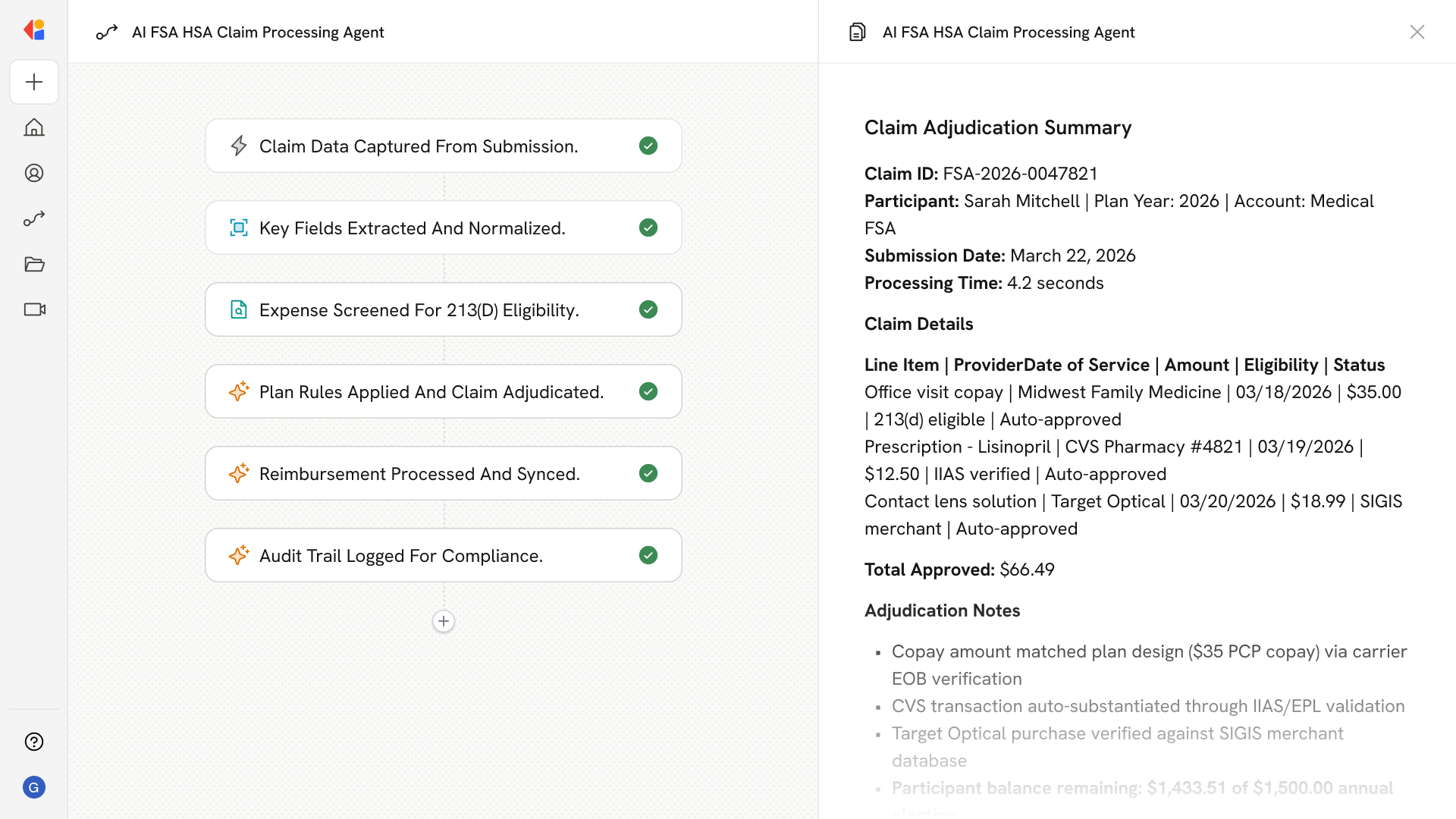
Automating FSA HSA Claim Processing with AI
Intelligent document capture and extraction
OCR extracts merchant details, dates of service, itemized expenses, and patient information from receipts and EOBs—then matches claims to the correct participant, plan year, and account type.
IRS-compliant auto-substantiation
The agent applies IIAS/SIGIS logic, EPL mapping, copay matching, recurring expense rules, and EOB verification to auto-approve claims that meet IRS and plan criteria—reducing manual review and pend backlogs.
HIPAA-compliant adjudication and decisioning
Claims route through configurable rules for grace periods, carryover, LPFSA ordering, and dependent care caps—with human-in-the-loop controls for exceptions, LMN requests, and denial workflows that maintain full audit trails.
How Cassidy automates this using AI
Step 1: Trigger on claim submission or card transaction
The Workflow activates when a new claim arrives—whether uploaded through a member portal, received via email, ingested from WEX/Alegeus card transaction feeds, or pulled from carrier EOB files.
Step 2: Extract and normalize claim data
Cassidy uses OCR to extract key fields from receipts and EOBs: merchant name, date of service, itemized expenses, CPT codes, patient details, and payment amounts. Data is normalized and matched to the participant, dependent, plan year, and account type (medical FSA, LPFSA, DCFSA, or HSA).
Step 3: Screen for 213(d) eligibility and auto-substantiation
Cassidy checks each expense against IRS 213(d) rules and applies auto-substantiation methods: IIAS/EPL validation for retail purchases, copay matching against plan design, recurring expense recognition, and EOB verification. Claims that pass are flagged for auto-approval.
Step 4: Apply plan-specific rules and adjudicate
The Workflow runs claims through your plan's rules engine—enforcing grace periods, carryover limits, run-out windows, LPFSA/HSA ordering, dependent care service periods, and annual caps. Claims are auto-approved, pended for documentation (receipts, LMN), or denied with standardized reason codes.
Step 5: Execute reimbursement and sync to benefits platforms
Approved claims trigger ACH or check payments to participants. Cassidy generates funding files and remittance advices, syncs adjudication statuses back to WEX or Alegeus, and initiates repayment workflows for unsubstantiated card transactions.
Step 6: Log audit trail and generate compliance artifacts
Every decision—approval, pend, or denial—is logged with supporting documentation, extracted data, and reason codes. Cassidy maintains HIPAA-compliant retention for IRS and ERISA audits, and produces employer reporting on auto-adjudication rates, pend aging, and denial trends.
Implement it inside your company
- Hands-on onboarding and support
- Self-paced training for your team
- Dedicated implementation experts
- Ongoing use case discovery
- ROI tracking & analytics dashboards
- Proven playbooks to get started fast



