AI Benefits Explanation Agent
Automating EOB Explanation for TPA Member Services with AI
Policy-Grounded, Line-by-Line Explanations
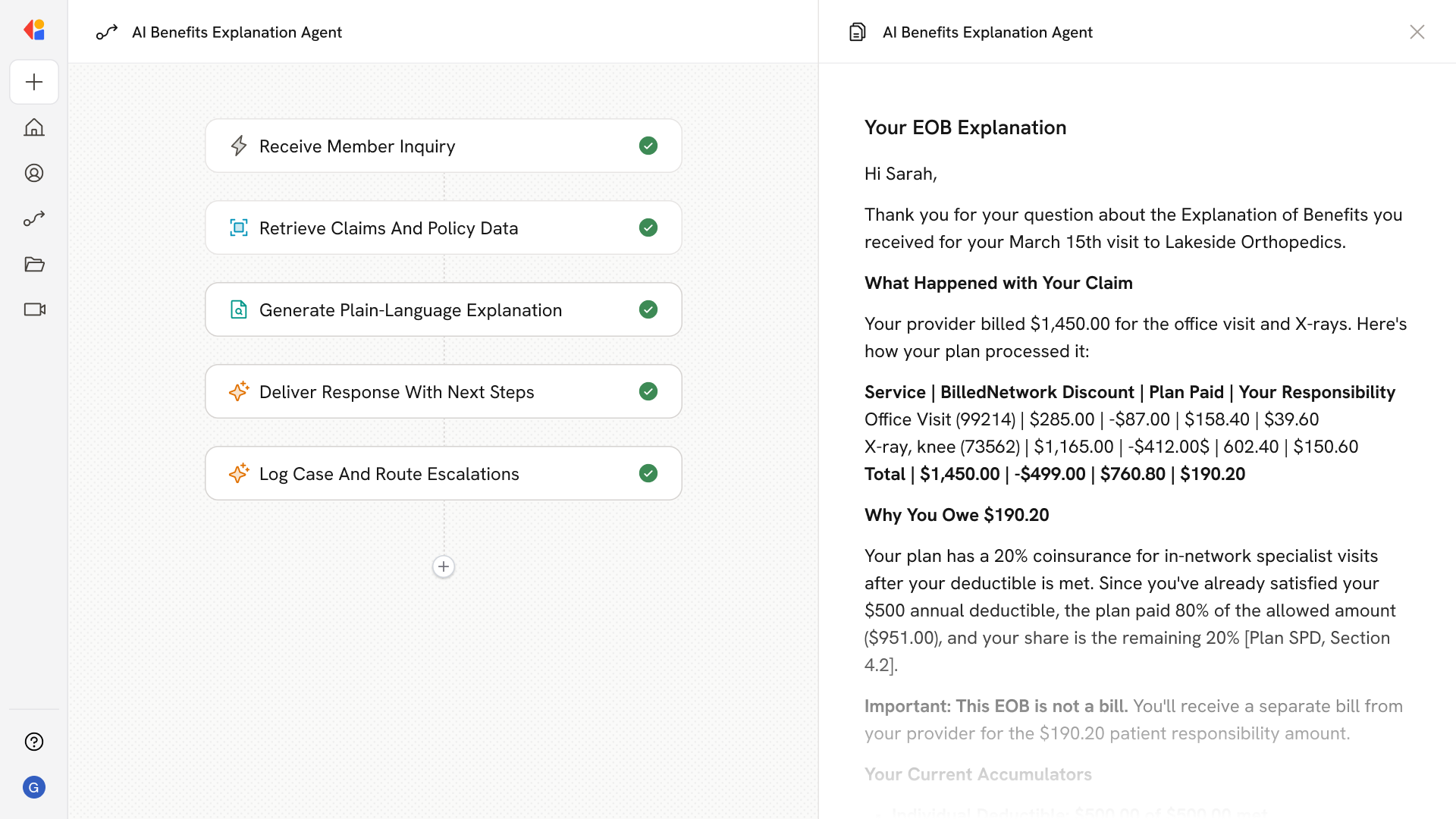
The agent retrieves claim details, CARC/RARC codes, and plan documents to deliver plain-language breakdowns of how billed amounts became member responsibility with citations to SPD sections and accumulator impacts.
HIPAA-Compliant, Authenticated Access
AI automation enforces role-based access controls, MFA verification, and audit logging to ensure PHI is only disclosed to authenticated members through secure channels meeting Minimum Necessary standards.
24/7 Resolution with Human Escalation Paths
Automated workflows answer member questions around the clock, then seamlessly route appeals, missing documentation requests, or complex COB scenarios to human representatives with full conversation context.
How Cassidy automates this using AI
Step 1: Trigger on member inquiry
The Workflow activates when an authenticated member submits a question through the portal chat, mobile app, or secure voice channel capturing the inquiry alongside verified identity credentials.
Step 2: Retrieve claims and policy data
Cassidy pulls the relevant claim lines, ERA/835 details, CARC/RARC codes, and current accumulators from the core admin system, then retrieves applicable SPD sections and coverage policies from the Knowledge Base.
Step 3: Generate policy-accurate explanation
The Agent reasons through the adjudication logic deductible application, coinsurance calculations, network discounts, and denial reasons to produce a plain-language explanation with line-item math and expandable citations to plan documents.
Step 4: Deliver response with next actions
Cassidy presents the explanation through the member's channel of choice, including deep links to the EOB PDF, clarification that the EOB is not a bill, and options to file an appeal, submit documentation, or connect with a human representative.
Step 5: Log case and route escalations
The Workflow creates a CRM case with the full conversation transcript, claim references, and member selections routing complex scenarios to appropriate queues while maintaining audit trails for HIPAA compliance.
Implement it inside your company
- Hands-on onboarding and support
- Self-paced training for your team
- Dedicated implementation experts
- Ongoing use case discovery
- ROI tracking & analytics dashboards
- Proven playbooks to get started fast



