AI Patient Admission Workflow Agent
Automating Patient Admission with AI
Eliminate Manual Data Entry and Duplicate Records
AI-driven patient matching and demographic standardization ensure accurate MRN assignment and clean data capture from the first touchpoint, minimizing costly reconciliation work downstream.
Accelerate Eligibility Verification and Financial Clearance
Real-time eligibility checks against payer systems confirm active coverage, benefits, and authorization requirements—enabling accurate cost estimates and point-of-service collections before the patient arrives.
Ensure Seamless EHR Integration and Care Team Notifications
Automated encounter creation and ADT messaging route verified patient data to clinical systems, ancillary departments, and care teams instantly, so registration never becomes a bottleneck.
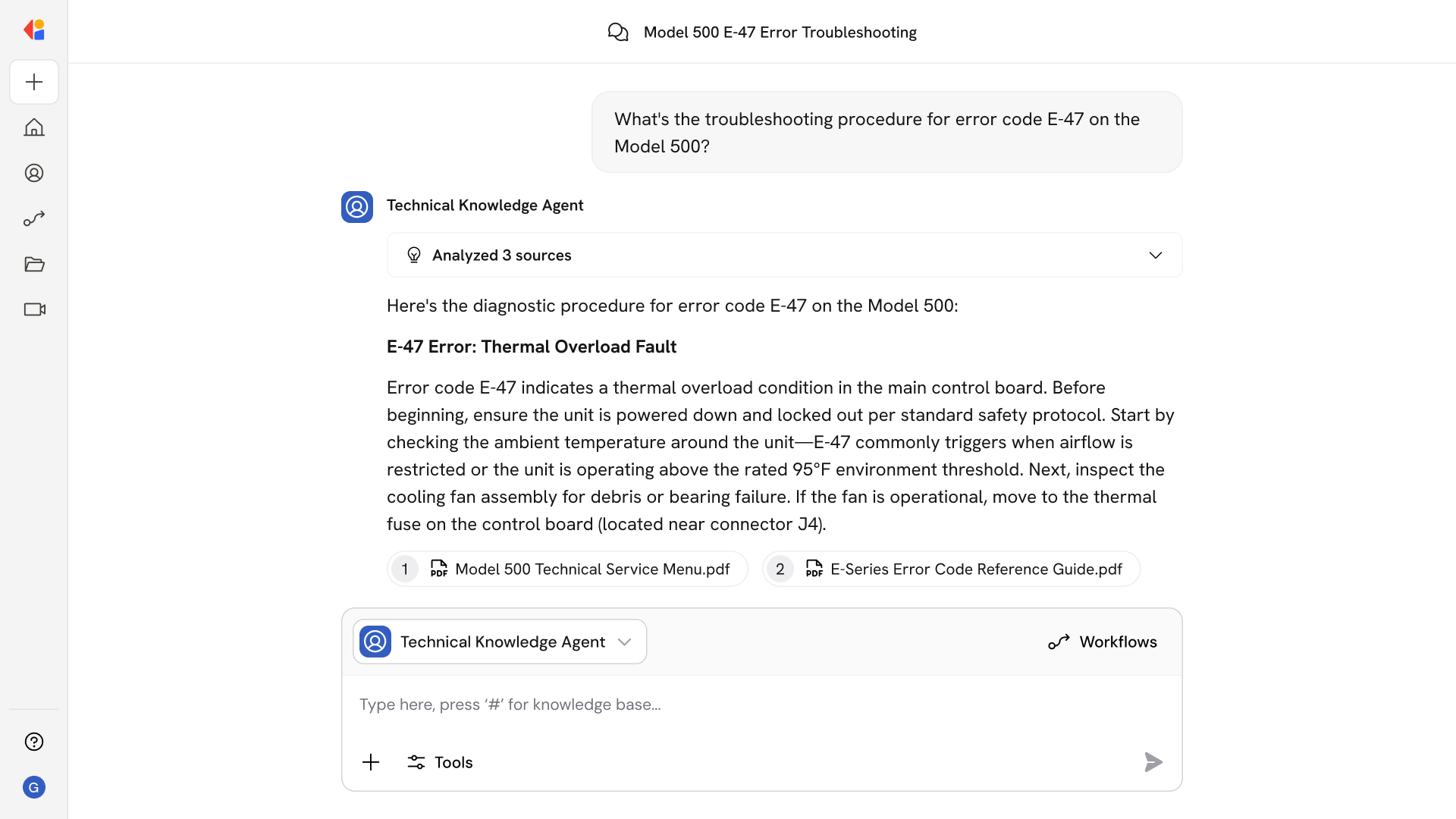
How Cassidy automates this using AI
Step 1: Trigger on new admission request
The Workflow activates when a patient admission is initiated—whether from a scheduling system, portal submission, referral interface, or front-desk check-in.
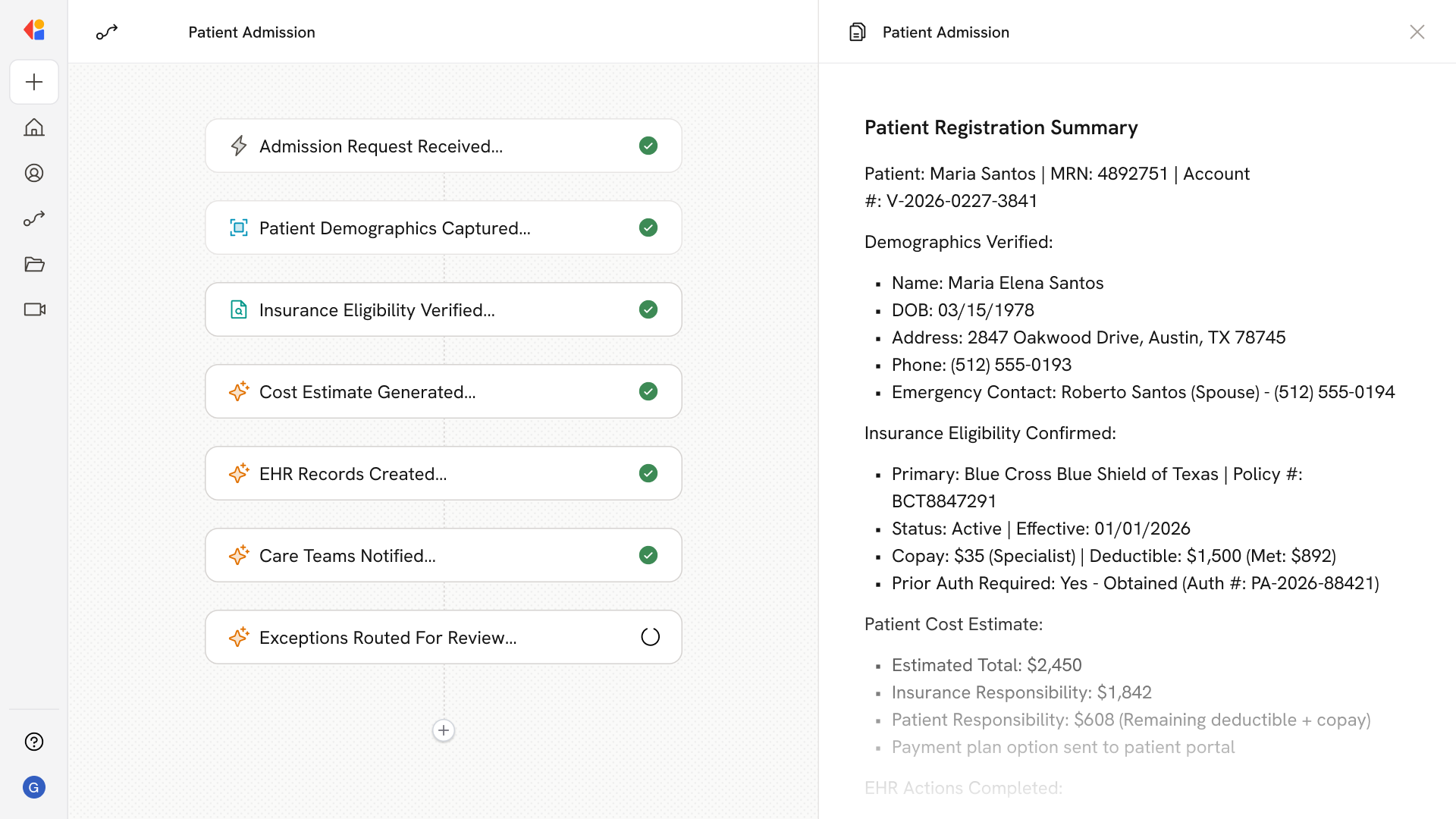
Step 2: Capture and standardize patient demographics
Cassidy extracts patient information from intake forms, scanned IDs, and insurance cards, normalizing names, addresses, and contact details to match your EHR's required formats and reduce duplicate record creation.
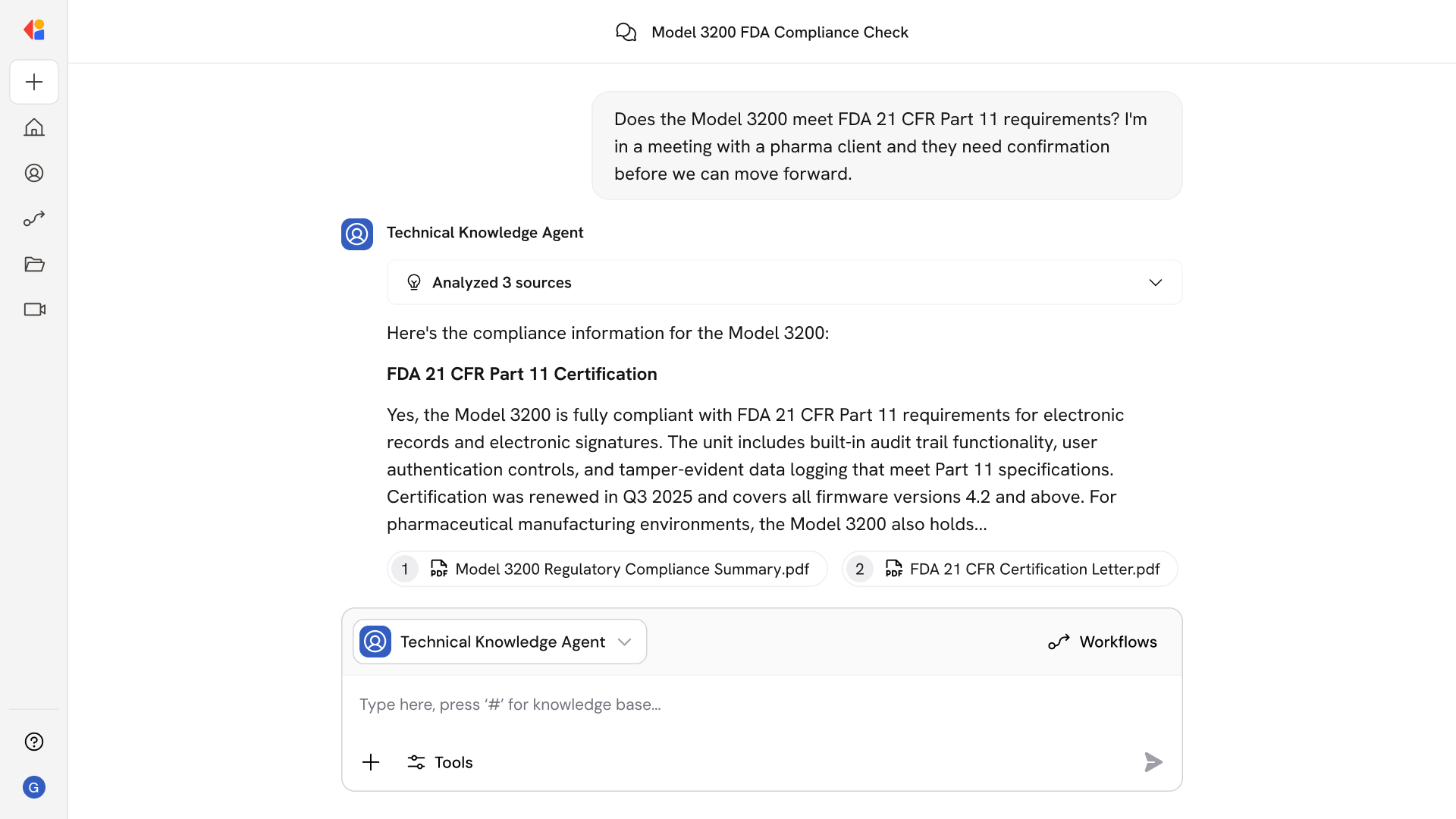
Step 3: Verify insurance eligibility in real-time
Cassidy queries payer systems and clearinghouses to confirm active coverage, plan details, copay and deductible amounts, coordination of benefits, and any prior authorization requirements.
Step 4: Generate cost estimates and flag financial clearance needs
Using eligibility results and contracted rates, Cassidy produces patient cost estimates, identifies charity screening needs, and routes accounts requiring payment plans or counseling to the appropriate work queue.
Step 5: Create or update patient and encounter records in the EHR
Cassidy creates the Patient and Encounter records with accurate MRN and Account/Visit Number assignments, attaching verified insurance data, scanned documents, and consent acknowledgments.
Step 6: Notify care teams and downstream systems
Once registration is complete, Cassidy sends ADT notifications to clinical teams, ancillary systems (lab, radiology, pharmacy), and capacity management—ensuring everyone has the information they need to begin care.
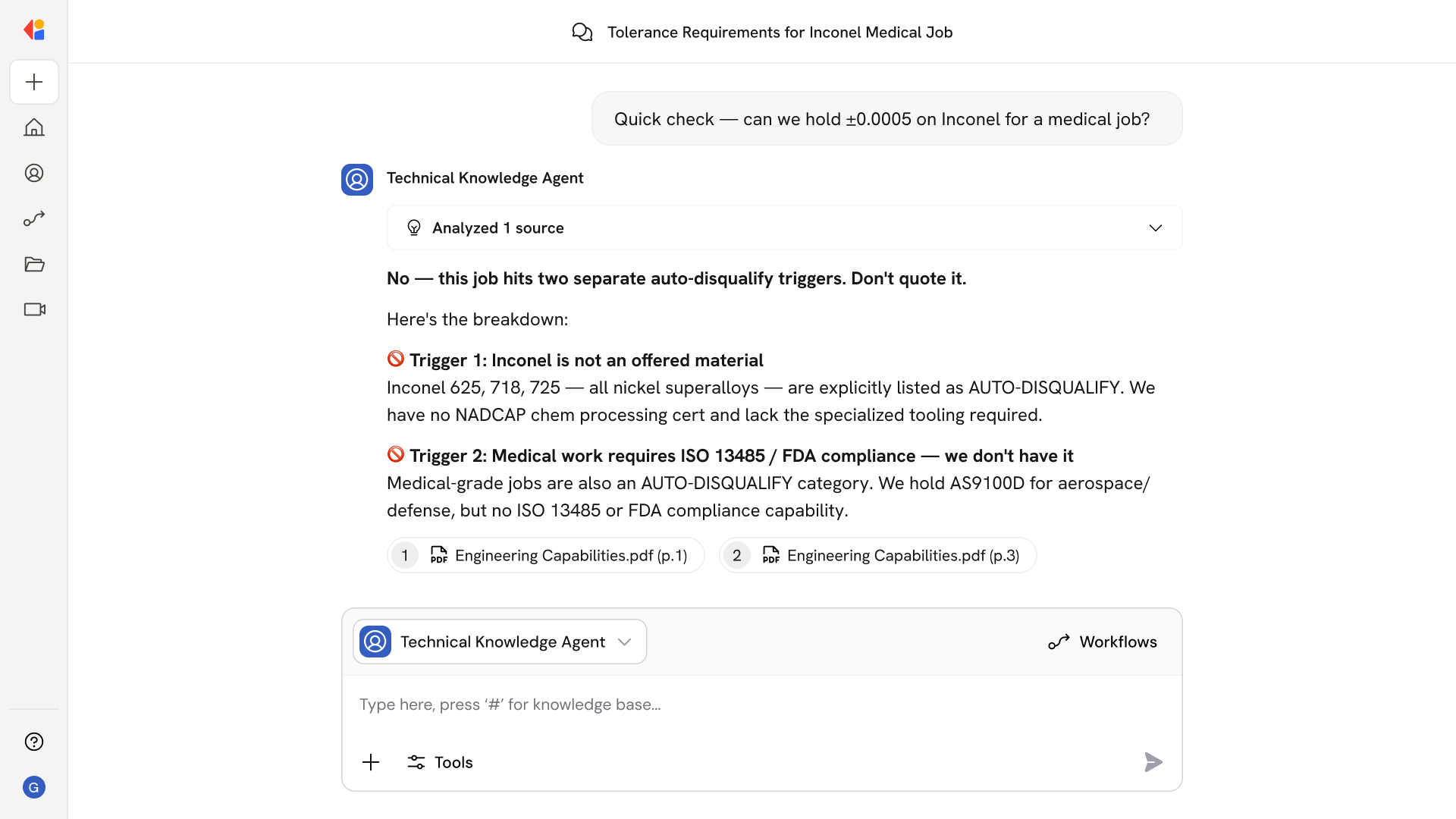
Step 7: Route exceptions for Human-in-the-Loop review
Identity mismatches, eligibility failures, or missing authorizations are flagged and routed to staff work queues with full context, keeping you in control of business-critical decisions while maintaining audit trails.
Implement it inside your company
- Hands-on onboarding and support
- Self-paced training for your team
- Dedicated implementation experts
- Ongoing use case discovery
- ROI tracking & analytics dashboards
- Proven playbooks to get started fast